A Steroid Treatment for COVID-19, and a Few Words About Steroids
As of this writing, the official global death toll from COVID-19 is 754, 185. However, ourworlddata.org (the source of this statistic) cautions: "the actual death toll is likely to be higher..."

Picture of masks used to create the GIF credited to: https://www.nursetogether.com/ Used under CC 4.0 license.

The COVID-19 deaths emphasize the urgency of finding a cure, treatment, and vaccine for this disease. Progress has not been encouraging. However, in recent months two drugs have proved helpful in very limited circumstances. Remdesevir, an anti-viral, and dexamethasone, a corticosteroid, have have been subjects of clinical trials and have been approved for use in severely ill, hospitalized patients. Other treatment options, such as plasma infusion and monoclonal antibodies are currently under review in clinical trials.
Researchers Looking at Slides of Cells that Make Monoclonal Antibodies

Image credit: National Cancer Institute, Linda Bartlett, Photographer. Public domain.

It may be surprising to readers that dexamethasone (the steroid) was actually more effective at saving lives than remdesevir (the anti-viral). This superior efficacy can be explained by what seems to be one of the most devastating consequence of a COVID-19 infection: widespread and severe inflammation. When it comes to stopping inflammation, steroids are the go-to medicine. However, their therapeutic action comes at a cost.
A Dachsund Suffering From Cushings Disease
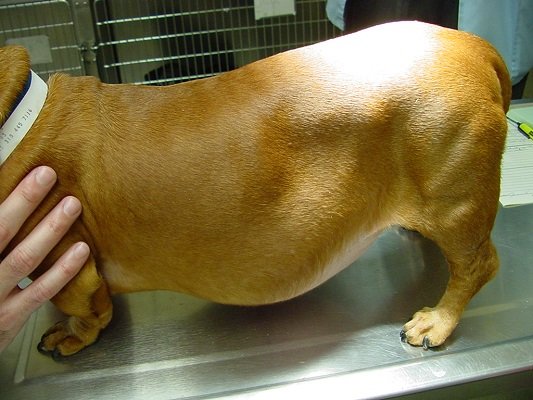
Picture credit: Self, CC 3.0. Cushings Disease results from too many steroids circulating in the bloodstream.

Most of us have probably been prescribed a steroid sometime in the past. Prednisone and hydrocortisone are two of the most commonly prescribed.
Use of the term steroid here should not be confused with anabolic steroids, the so-called performance-enhancing drugs. Anabolic steroids mimic the action of a sex hormone, progesterone. Dexamethasone, and other therapeutic steroids referred to in this article, are corticosteroids and mimic the action of cortisol. Cortisol is a naturally occurring, essential hormone released by the adrenal glands. This hormone is involved in regulatory functions throughout the body and is integral to the HPA axis.
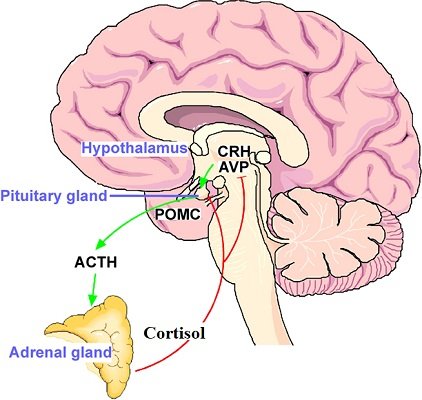
Picture credit:Murgatroyd C and Spengler D (2011) Epigenetics of early child development. Front. Psychiatry 2:16. doi: 10.3389/fpsyt.2011.00016 http://journal.frontiersin.org/article/10.3389/fpsyt.2011.00016/full
CC 3.0 license

Cortisol is often referred to as the 'stress' hormone but its effects in the body are more far-reaching and profound than that. Because of these far-reaching effects, taking a synthetic steroid can have serious, and even, in some cases, life-threatening consequences.
Osteoporosis Is One Common Side Effect of Steroid Treatment
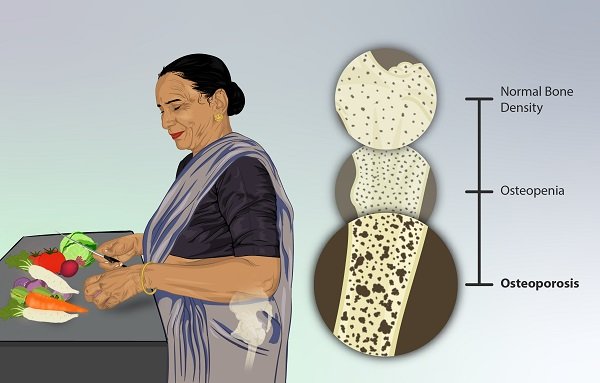
Picture credit: https://www.myupchar.com/en/disease/osteoporosis. Used under CC 4.0 license. The caption under the picture reads: "This is a depiction of a woman suffering from Osteoporosis. The loss of bone mass has been shown, in comparison to Osteopenia (a milder condition) and a normal bone".

Dexamethasone as an Anti-Inflammatory
Dexamethasone, as a cortisol-mimicking steroid, is a powerful anti-inflammatory. It's an established treatment for a number of inflammatory conditions, including: "severe allergies, some types of nausea and vomiting, arthritis, swelling of the brain and spinal cord, severe asthma, and for breathing difficulties in newborn babies." 1 The anti-inflammatory action of dexamethasone has been found to curb some of the most severe ravages of COVID-19.
 When Is Treatment with Dexamethasone Appropriate?
When Is Treatment with Dexamethasone Appropriate?
In the use of dexamethose for treatment of COVID-19, "timing is everything". How would a doctor know just exactly when the right time was? Happily, there is actually a test.
A Drawing of C-Reactive Protein: Important in COVID-19 Treatment
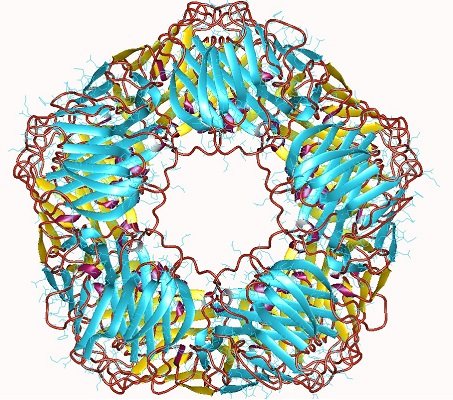
Picture credit: Ramadan, M.A., Shrive, A.K., Holden, D., Myles, D.A., Volanakis, J.E., DeLucas, L.J., Greenhough, T.J.; Visualization author: User:Astrojan, Used under a CC 3.0 license.
C-reactive protein is a marker for inflammation.

A June 2020 article in Science explains that in one study, mortality in severely ill COVID-19 patients was reduced by 30% when dexamethasone was administered. However, another report, published in the July/August issue of the Journal of Hospital Medicine describes findings that show patients may actually be harmed if dexamethasone is administered. The difference? Dexamethasone is helpful only in the late stages of the disease, when inflammation is causing great harm. In the early stages, before patients are very ill, use of this steroid will actually result in a higher rate of death.
 C-Reactive Protein Is Key
C-Reactive Protein Is Key
This blood test looks for inflammation anywhere in the body. C-reactive protein is often part of a routine blood panel. An elevated level means there is inflammation somewhere in the body. The higher the level, the greater the inflammation. Thus, C-reactive protein is an excellent screening tool for administration of dexamethasone.
One Potential Side Effect of Steroid Treatment: Diabetes
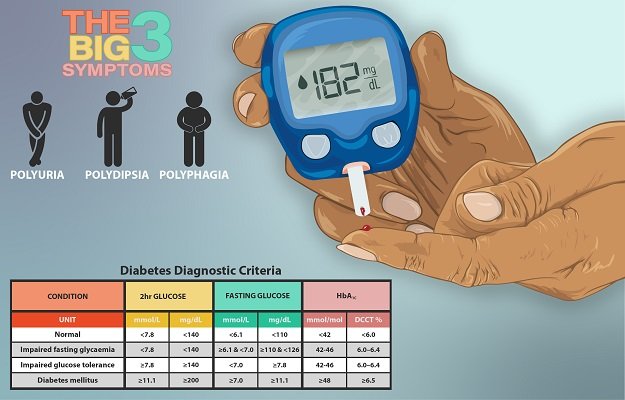
Picture credit:https://www.myupchar.com/en/disease/diabetes. CC 4.0 license
In a patient who is severely ill and experiencing diffuse inflammation, dexamethasone could be a life saver. However, in a patient who is not severely ill and who is not experiencing high levels of inflammation, dexamethasone might actually reduce the body's ability to fight infection. This would give the virus an opportunity to grow stronger and might actually result in the patient's death.
The importance of C-reactive protein as a screening tool was explained in a Journal of Hospital Medicine article. The article cites an 'observational' study which showed levels of C-reactive protein correlated with successful steroid treatment. The article states that in patients with a C-reactive protein (CRP) finding equal to or greater than 20mg/dL, use of the steroid reduced probability of death or mechanical ventilation 'significantly'. However if the CRP reading is less than 10mg/dL, then treating with steroid "increased the risk of death or mechanical ventilation".
While this result seems compelling, the article hastens to caution that more clinical trials are needed to make certain these results hold up.
A Certain Type of Cataract is Associated with Therapeutic Steroids
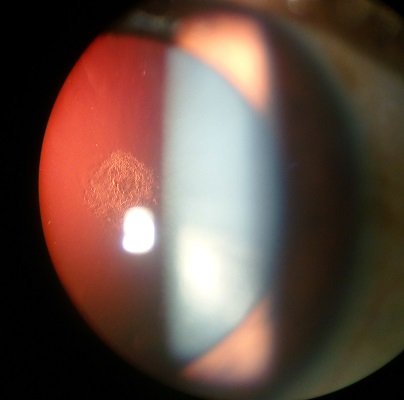
Image credit: Imrankabirhossain. Used under a CC 4.0
The type of cataract shown in the image above, Posterior subcapsular cataract, is associated with steroid use.

Other Steroid Formulations May Also Be Helpful in the Treatment of COVID-19
A study, performed at the Albert Einstein College of Medicine and Montefiore Health System indicated that commonly prescribed steroids, besides dexamethasone, have been helpful in treating patients who are severely ill with COVID-19. The drug mentioned in the article is prednisone.
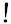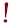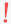 Paradox of Corticosteroids
Paradox of Corticosteroids
The paradox at the heart of steroid therapy for COVID-19 is a challenge that confronts every physician who prescribes steroids for any condition. That paradox confronts patients who must decide in many cases whether the steroid is going to do more harm than good.
Many people who take corticosteroids are unaware of their potential complications. The drugs are so frequently and casually prescribed that patients may be complacent about the serious nature of the drug.
Steroid Therapy May Cause Fatty Live
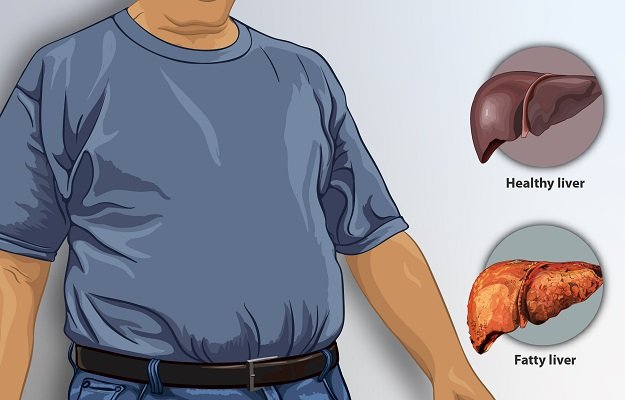
Picture credit:https://www.myupchar.com/en/disease/fatty-liver. Used under CC 4.0 license
The casual approach many doctors, and patients, take toward steroids is addressed in a 2016 Rheumatology article: "physicians have somehow become inured to the harmful long-term effects of glucocorticoids in patients", the authors of the article state.

 A Personal Choice
A Personal Choice
I take prednisone every day. This was a decision I came to reluctantly. I weighed the drug's benefits and risks. The benefits I have described already in this blog. It is a powerful anti-inflammatory. I've mentioned several of the risks. The list is really quite long and if you are confronted with the possibility of taking therapeutic steroids, you should be aware of these. This will not only help you to come to a decision, but will also help you to monitor yourself for possible side effects.

Steroids Have Such a Wide-Ranging Effect Because They Are Pleiotropic
Corticosteroids have therapeutic qualities, but it is not a targeted therapy. The effects can be experienced in organs and tissues far removed from the area of interest.
 Organ Damage
Organ Damage
We have established so far in this blog that corticosteroids cause organ damage. At what dose, for what duration, which organs? It would be nice to know, to have a fast rule. Unfortunately, researchers are not in complete agreement about how much, how long, who and when this damage will occur. One thing just about all researchers agree on: harm, if and when it does occur, is dependent upon dosage level and duration of treatment.

Image credit: National Cancer Institute, Unsplash. Public domain
The more steroid a patient takes, the longer it is taken, the greater the chance of organ damage. Two reports demonstrate the conundrum facing physicians, and patients, as steroid therapy is considered:
- A 2009 article in the Journal of Rhuematology finds: "Compared with no prednisone use, the increase in risk is small or nonexistent for a cumulative average dose below 180 mg/month "
- The authors of a study published in Rheumatology (Oxford Academics) found that: " no safe dose of glucocorticoids exists ". Although later on in the same report these authors also find evidence of little organ damage at doses under 7.5mg per day, or 5mg per day.

Suppression of the HPA Axis: Adrenal Atrophy
One of the major risks of steroid therapy is suppression of the HPA axis. The body will fail to produce cortisol on its own and therefore the patient may need to take steroids for life. This is a risk that can be underappreciated particularly at time of great stress, such as during and after surgery. Or even during illness.
Cortisone Injection for Tennis Elbow
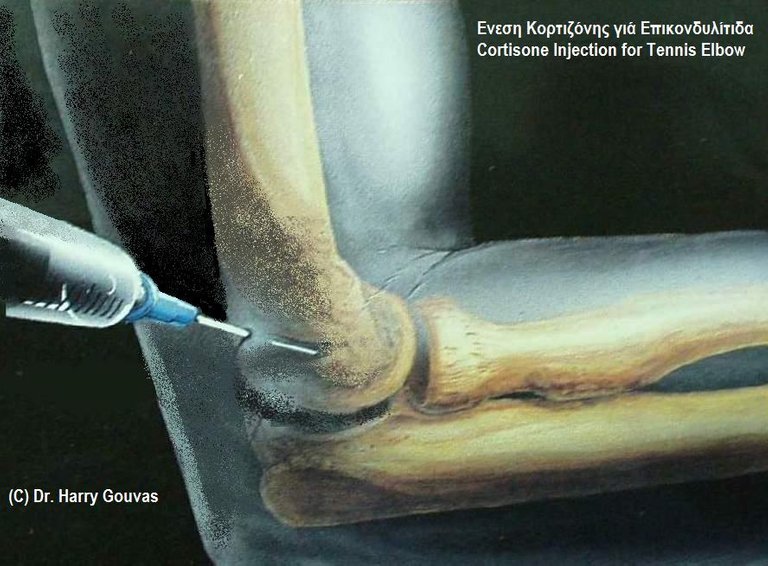
Image credit: Σχέδιο: Δρ. Χαράλαμπος Γκούβας (Harrygouvas) CC 3.0 license
Ordinarily the body would release extra cortisol to handle increased stress. In cases where a patient has taken steroids, perhaps even within the past year, a doctor will have to administer supplemental corticosteroids in order to meet the stress demands occasioned by surgery. This may also be true for people who have received steroid injections for painful joints. Failure to take proper precautions when undergoing surgery could result in a crisis, and even death.
 Mitigating HPA Suppression
Mitigating HPA Suppression
Patients can help to minimize HPA suppression by taking their medication in the morning, by only taking one dose a day, and, if possible, by taking the dose on alternating days. These methods seem to encourage the adrenal glands to continue producing cortisol.

*Conclusion
There's so much more to say, but this is enough of a review to apprise readers of the benefits and risks of corticosteroids. It is my opinion that it is a mistake to leave all decisions about the drug to a physician. An article in the Journal of Clinical Research Medicine discusses some of the reasons doctors might prescribe, or over prescribe, a steroid. One reason is to cut back on phone calls and paper work from patients who do not see quick results, or who are uncomfortable. A quote from the article, which suggests prescribing a higher dose of prednisone: "the benefits of convenience for the patient and less work output in the form of repeat phone calls, visits, and nursing/physician time."
I hope this wasn't too tedious, and more importantly, I hope if any of my readers are prescribed dexamethasone or any other corticosteroid that this information may be helpful. Meanwhile, be well.


Sources
1.Our World Data.org
2.NIH
3.NEJM
4.Drugs.com
5.Statnews.com
6.NBCnews.com
7.Miragenews.com
8.Sciencedirect.com
9.Myupchar.com
10.The Conversation
11.Rebelem.com
12.Mayoclinic.org
13.Science
14.Journal of Hospital Medicine
15.Journal of Hospital Medicine
16.NCBI.NLM.NIH.gov
17.USA Today
18.Rheumatology
19.Wikipedia/Drugs
20.Proquest.com
21.Journal of Rheumatology
22.Rheumatology
23.Uptodate.com
24.Wikipedia.org/adrenal insufficiency
25.NCBI.NLM.NIH.gov/books
26.Journal of Clinical Research Medicine
27.Everydayhealth.com
28.NBC News.com: Brain Inflammation
29.News Medical.net
30.NEJM Steroids and Cataracts
Footnote:
1 The Conversation: Desamethasone, the Cheap, Old and Boring Drug That's a Potential COVID-19 Treatment
Upvoted by GITPLAIT!
We have a curation trial on Hive.vote. you can earn a passive income by delegating to @gitplait
We share 80 % of the curation rewards with the delegators.
To delegate, use the links or adjust 10HIVE, 20HIVE, 50HIVE, 100HIVE, 200HIVE, 500HIVE, 1,000HIVE, 10,000HIVE, 100,000HIVE
Join the Community and chat with us on Discord let’s solve problems & build together.
The Covid fanfare has died down now. At some point, people won't even care anymore and will just go about their lives. Whatever happens, happens
Posted using Dapplr
In the U.S. we're averaging about 1000 deaths from COVID a day. That's down a bit, but schools and businesses are reopening and predictions are that we will inevitably see an uptick.
The head of the U. S. CDC says the fall will be brutal--"the worst we've ever had". I'm glad that wherever you live COVID is not an issue. Where I live, in New York, we lost many when the virus raged a few months ago, Some of these people I actually knew. It's quieter now in New York, but we are watchful.
People get used to anything. Psychologically they can't live in a perpetual state of crisis. They get used to war, and hunger. But just because people are weary, doesn't mean the danger of these conditions has evaporated.
Thank you for your comment. I love comments. Let's me know how the blog hits people. I work really hard on these and comments are my reward.
Have a great day, and be well.
It's the same in most parts of the world. At the beginning, when the virus wasn't even as rampant as it is now, people were more scared and shit.
The media and anybody that wanted some attention rode the wave and used it for clout. The biggest irony is that when it is already spread out, they're talking about opening schools and shit.
Yes. A tragic irony that will cost lives.
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider supporting our funding proposal, approving our witness (@stem.witness) or delegating to the @stemsocial account (for some ROI).
Thanks for using the STEMsocial app and including @stemsocial as a beneficiary, which give you stronger support.
Thank you very much. Really makes my day when I know I've met STEMsocial's standards. I appreciate the support :)
Congratulations @agmoore! You have completed the following achievement on the Hive blockchain and have been rewarded with new badge(s) :
You can view your badges on your board And compare to others on the Ranking
If you no longer want to receive notifications, reply to this comment with the word
STOPTo support your work, I also upvoted your post!
Do not miss the last post from @hivebuzz:
Thank you for this well researched information!
Thank you very much :)
Thanks for all your information. I have a family member who takes prednisone daily. It is a risk-reward medication. Great job.
Thank you for your response. I'm glad the information was meaningful to you.
Dear AG,
Thank you so much for your elaborately and well researched article! I hope that many people concerned will read the information.
Personally, I take an asthma spray from time to time, which contains budesonide, an active substance that belongs to the glucocorticoid group. During my last eye checkup, the doctor already noticed slight damages in my eyes, which he attributes to this medication. That makes me think.
All the best for you. Be well and safe,
Affectionately,
Anna
Dear Anna,
Thank you for your kind words, but I was distressed to read about your eyes. The connection between inhaled steroids and organ damage (including the eyes) is under investigation. I hope you don't mind that I looked up a few articles. This is something I wanted to cover in the blog but people have limited patience so I had to cut the piece down.
Here's an article from 2019 that describes a subset of patients with chronic asthma who might be able to take a non-steroidal medicine and receive the same benefits. Apparently it has something to do with the amount of eosinophils in sputum. The doctor can test for this. So, it might be something for you to look into.
There are links between inhaled steroids and glaucoma.This article is from 2018 so it is fairly recent. The study does show that there is only an association with glaucoma at higher doses of inhaled steroid.
There seems to be less of an association between inhaled steroids and cataracts, according to this 2020 article from The Journal of Allergy and Clinical Immunology
Hope you don't think I'm presumptuous. Years ago I had great difficulty with an autoimmune disease and learned that educating myself was the best way toward a better quality of life, so I try to share information whenever I can. Then if something goes wrong, I can't blame the doctor because I had a hand in deciding my treatment plan :)
Please be well. I do appreciate your stopping by my blog.
Affectionately,
Your friend from New York who does not want winter to come
AG
Dear AG,
I'm very grateful and appreciate that you have looked up relevant articles for me. I have printed / saved the publications and will study them in peace. Luckily I don't have to use the spray regularly, but only during the allergy season mainly in spring.
How could I find you presumptuous? On the contrary, you show me how a responsible patient should act. Namely not to put fate solely in the hands of doctors, but to inform yourself and participate in the therapy plan.
Thanks once again and have a cozy and peaceful Sunday. Winter can wait! Let's first still enjoy the beautiful late summer days.
Affectionately,
From sunny Vienna,
Anna
🌞🌷 🌸 🌺 🌞
How detailed! I am pinning this as a model example to some newer kids on the StemSocial block struggling with quality and personality!
Nice to see you around as always =)
PS: I'm pretty sure that fatty liver image is modeled off mine
Thank you very much @mobbs. It took me a while to get this out. I had so much material that I needed to find a focus. Also, we had widespread power outages here (Isaias) so that slowed me down. But in the end, I spent so much time with the piece that it almost wrote itself.
I really appreciate your high praise, and very much appreciate STEMsocial's support. Basically, I blog here and on LMAC. Doesn't seem to be time for much else. Plus these two communities are very congenial. Important to me.
Hope you and your lovely cats are well--and I don't believe that bit about the fatty liver :))
AG
This is quite informative and well researched. I can imagine the amount of time spent on this for it to have such amount of information.
I never knew dexamethasone could have such a debilitating effect. Why is it then available over the counter? I remember vividly it's one of the easily accessible drugs without prescription when I was working as pharmacy technician a few years back.
BTW what are the requirements for carrying out the C-reactive protein test? Just wondering if we've got those around here.
In the U.S. you can't get oral corticosteroids without a prescription. I don't think you can get an inhaler, either. It is possible to buy a very low strength topical, and these even cause difficulty because they are absorbed through the skin. I can't believe such powerful medications are available over the counter. Amazing.
Thank you for the kind words. Yes, there was a mountain of research. One of the hardest parts was deciding what to leave out. My son thinks I should do a part 2, which could be helpful in identifying the different names under which the drugs are sold and the equivalencies of the drugs. So much I left out here.
Hope you and your family are well.
Regards,
AG
Edit:
Here's an article that describes methodology for the C-reactive protein test. Hope the article is helpful.
Great information! took me some time to go through it but worth reading. Steriods have never been so healthy and side effects is the added bonus with it.
I wonder @agmoore how old are you, Sir! Did your physician prescribe you prednisone?
Hello @razeiv,
Thank you for stopping by. Yes, the material was quite extensive, but I hoped to give people some important information.
How old am I? Quite old, over 70! Some might think too old to be playing in the fantasy world of LMAC, but I am proof that the imagination lives, and is even freer as we grow older...if only we give it a chance to breathe :)
In the U. S. we cannot buy prednisone without a prescription. I had to be talked into this, and coaxed by circumstances. However, sometimes, there are no great choices and I was lucky that this worked for me and so far (years now) at a low, low dose no serious consequences.
Well, I'm working on my #LMAC blog. Finished the collage and just writing a bit to go along with it. I have to catch up with my friends over there. So busy with the science blog I've been distracted.
See you at LMAC, soon :)
Oh I see .. No dear we are never too old to imagine. Still, a lot more to go for you, 70 is just the beginning, I'm certain :D
I'm on it too, let's see if I can finish it quick. Also, excited to see what's in your bucket of ideas this week :D
Hello @agmoore, thanks for your well elucidated writeup, i enjoyed every single bit of it. Absolutely beautiful, it is worth mentioning that steroids may not only induce cataract formation in the eye but also increase intraocular pressure which could lead to glaucoma formation especially for topical steroids. Thanks for well informing us.
Hello @nattybongo,
Thank you for those kind words. I've looked up a couple of articles about topical steroids and glaucoma (since I read your comment) and it is something I'd like to look into more. One thing I discovered is there are three categories of patients who take steroids: high responders, moderate responders and non-responders. This article explains different reactions to steroids. Fascinating. I guess it would be good for a patient and doctor to know which catergory the patient fits into to assess risk.
Thanks for that informative response. I love it when more questions are raised...that is, stuff I don't know.
Be safe and well, @nattybongo
Regards,
AG
I am subscribed to the Conversation, and had blogged some of their articles on my website, but somehow missed this one. I am appreciative of the fact that these are published under a CC License. Some of their articles I published here: CORONAVIRUS BLOG.
Related video:
Thank you! I will look into that.
Regards,
AG