Risk Factors for Glaucoma
Greetings to all and sundry,
It is a beautiful day today, the week has started right for most of us and things are going as planned, I am optimistic that we will all end the week on pleasant notes, I am just happy that I get the opportunity once again to share with you some insights into the eye, its related pathologies and general care.
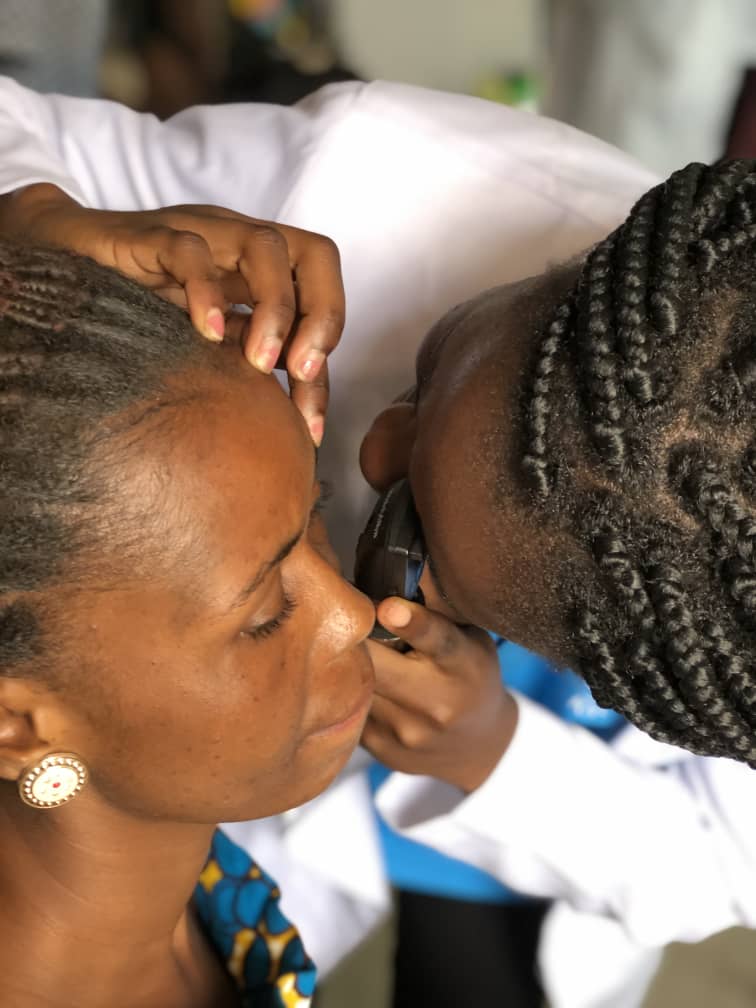
For this week I have been focusing on Glaucoma and I would be continuing with this today too. I am optimistic that by the time we are done talking about glaucoma, you would have learned a whole lot, perhaps not enough to be an expert but enough to understand the intensity or severity of the condition. I am also doing this because the 12th March to 18th of March has been internationally dedicated to Glaucoma awareness.
And so with the aid of this platform and our science community, I wish to contribute my quota to the awareness program by sharing what I know with all of us. I do hope you continue to enjoy what I have to share with you. Ok, so let's get one with what we have to learn today.
Introduction
A quick recap, in our previous two discussions on Glaucoma we came to learn what Glaucoma is and we understood that it is a degenerative condition of the eye which involves atrophy of the optic nerve which mostly comes about with an increase in intraocular pressure and characteristic visual field loss. But then we also learned that this may not always be the case one could have glaucoma and still have normal ocular pressure.
This was classified as normal-tension glaucoma, we also learned that in these cases the apoptosis of the cells seems to be idiopathic and the cascade continues as one cell's death triggers the next. We also looked at some of the myths about glaucoma which included the fact that glaucoma has no cure and so we would have to get ourselves checked because early detection is what saves the sight. And then we talked about the fact that glaucoma is not a condition that is only seen in adults but could apply to anyone including babies born today.
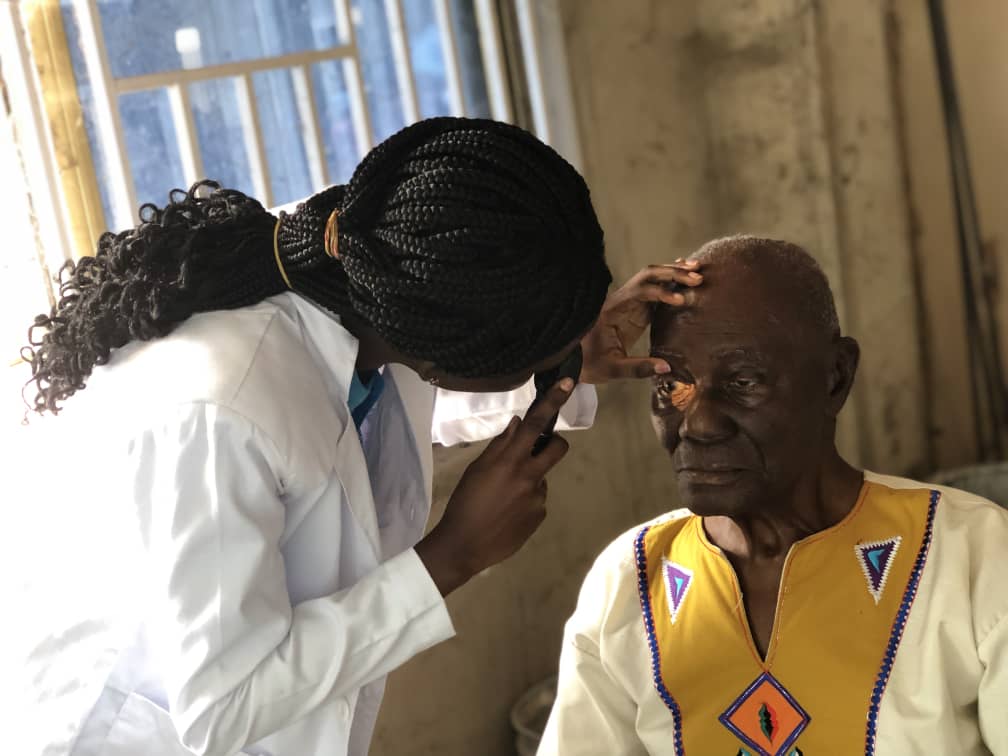
We also said glaucoma doesn't give any symptoms and so your headaches or pain, burning sensations, photophobia, and other discomfort you are experiencing are not a result of glaucoma but there are signs which could help your Optometrist detect glaucoma and this is best observed with clinical tools and equipment, which is why a regular eye examination is important.
Before we move on to today's risk factors though I'd like to add a few myths which came up. It is worth noting that spectacles ain't a solution to glaucoma, glaucomatous damages ain't reversible and spectacle wouldn't do much if any to improve your vision if the loss is a result of glaucomatous damage. If vision is quite down, you may need low vision aids and so your Optometrist may refer you to another specialist for that. And please note that glaucoma is not contagious, you can't contract glaucoma through any physical, there are however genetic factors to consider and so if a sibling is diagnosed it would be important to get yourself checked.
Risk Factors
Like most conditions, some predisposing factors may make one more susceptible to acquiring or developing the condition, and knowing if you fall within these risk factor groups helps get yourself checked as well as have routine checkups. But then, even if you do not fall within these categories please do have regular eye examinations, it may not be glaucoma but other ocular conditions are also sight-threatening and early diagnosis may save your sight.
- Heredity/Genes
Let's begin with the familiar, by now if you have been following me on this you are probably aware of the fact that glaucoma has genetic implications and that your relative having the condition makes it a risk factor for you and you would have to get yourself check out as soon as possible. From personal experience, I can tell you that the condition can sometimes skip generations and so you do not have to be alarmed just yet.

The fact that your mum or sister was diagnosed with glaucoma doesn't necessarily mean that you have the condition or that you will develop the condition, it simply means you have to take good care of your sight and have regular checkups because there is that possibility. Note that more research is being done in this area and we would probably know more in the years ahead.
- Age and Gender
Vision scientist would tell you that annually we lose some number of optic nerves with or without glaucoma but then you realize that as we age our intraocular pressure generally seem to increase a little and this may be attributed to the fact that our ocular structures get weaker and become less efficient as we grow which directly or indirectly affect aqueous productions as well as its drainage.

Then when you go further down this line you will also come to learn that whiles our eye pressures become a bit elevated as we grow older, it tends to be higher in women as compared to men and so statistically you may find more women with the glaucoma condition as compared to men. But then it could also be because women's population over shadow's that of men? Either way, understanding where you fall would do you a lot of good in protecting yourself or better still doing the needful.
- Systemic Conditions and Race
Some conditions may make it easier to develop glaucoma as you age due to the effects it tends to have on the eye. For instance, diabetes has the tendency of causing cataracts, weaken blood vessels, and block drainage outflows which could eventually cause a gradual rise in ocular pressure leading to glaucoma. Again, a lot of glaucoma patients tend to be hypertensive too.

Currently, Africa seems to have a very high prevalence of open angle glaucoma whereas close-angle glaucoma is more seem among people of eastern descent. Latinos also happen to have a higher propensity to developing glaucoma similar to that of Africans and African-Americans.
- Drugs and Habits
The last things I would be talking about are our habits and the things we consume. Scientists found that people who are more active and athletic, do work out and all tend to have lower intraocular pressures as compared to individuals who have more of a sedentary life. There's there is also the part about drugs.

People who may be on steroids for a long time would more likely have a higher intraocular pressure, taking caffeine as well as smoking is also known to increase intraocular pressure whereas alcohol and drugs such as timolol which are antiglaucoma drugs do well in reducing the pressure. But please do not become an alcoholic if you are diagnosed with glaucoma because you want to lower your Intraocular pressure, it is the wrong way to go about it. See your Optometrist for proper management and guidance.
Conclusion
Glaucoma is real and people are losing sight of this condition on a daily, until you perhaps see it happen you may not believe it but take it from me because I see patients on a daily and I know how dicey things can get with glaucoma as a condition. And so please do right by yourself and with your eyes, get yourself checked today, glaucoma test doesn't take more than a few minutes.

You do not need to have any issues before you visit your Optometrist, you can walk in any day for a check I would also advise you to take advantage of this week's awareness creation and participate in the free screening programs being organized all around, get your eyes checked today, your future self may thank you for those few minutes you spent at the office of your Optometrist. It was a pleasure serving again today and I look forward to being able to do more.
Further Reading
Coleman, A. L., & Miglior, S. (2008). Risk factors for glaucoma onset and progression. Survey of ophthalmology, 53 Suppl1, S3–S10. https://doi.org/10.1016/j.survophthal.2008.08.006.
McMonnies C. W. (2017). Glaucoma history and risk factors. Journal of optometry, 10(2), 71–78. https://doi.org/10.1016/j.optom.2016.02.003.
Schuster, A. K., Wagner, F. M., Pfeiffer, N., & Hoffmann, E. M. (2021). Risk factors for open-angle glaucoma and recommendations for glaucoma screening. Risikofaktoren für das Offenwinkelglaukom und Empfehlungen zur Glaukomfrüherkennung. Der Ophthalmologe : Zeitschrift der Deutschen Ophthalmologischen Gesellschaft, 118(Suppl 2), 145–152. https://doi.org/10.1007/s00347-021-01378-5.
Song, B. J., Aiello, L. P., & Pasquale, L. R. (2016). Presence and Risk Factors for Glaucoma in Patients with Diabetes. Current diabetes reports, 16(12), 124. https://doi.org/10.1007/s11892-016-0815-6..**
European Glaucoma Society Terminology and Guidelines for Glaucoma, 5th Edition. (2021). The British journal of ophthalmology, 105(Suppl 1), 1–169. https://doi.org/10.1136/bjophthalmol-2021-egsguidelines.
Ng, J. K., & Lau, O. (2022). Traumatic Glaucoma. In StatPearls. StatPearls Publishing..
Esporcatte, B. L., & Tavares, I. M. (2016). Normal-tension glaucoma: an update. Arquivos brasileiros de oftalmologia, 79(4), 270–276. https://doi.org/10.5935/0004-2749.20160077.
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider delegating to the @stemsocial account (85% of the curation rewards are returned).
You may also include @stemsocial as a beneficiary of the rewards of this post to get a stronger support.