HEALTH AND DISEASES: Detailed Explanation on Different Types of Cardiovascular Disease.
Cardiovascular disease is a general term. The symptoms and effects of different forms depend on which blood vessel is affected. The severity of the condition depends on the extent to which the vessel is blocked, Generally, partial blockages in small arteries or veins are less life-threatening than complete blockage of a major vessel. A summary of different forms of cardiovascular disease is given below.
Heart attack
An heart attack, or myocardial infarct, happens when the blood supply to the heart muscle is interrupted. The cause of the interruption is usually a blockage of one of the coronary arteries. This can be due to a blood clot that has travelled to the heart from elsewhere in the body, or it can be due to atherosclerosis. When blood cannot get oxygen to the heart muscle, the affected part of the heart dies. An heart attack causes severe pain in the chest and left arm. Mild heart attacks are dangerous but do not kill; careful treatment using drugs to 'thin' the blood to prevent another blockage, followed by a change in lifestyle can help to prevent another attack.
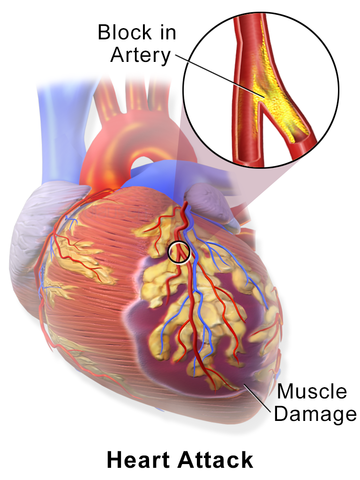
Summarily, an heart attack occurs when the coronary arteries become blocked by an atheroma or by a blood clot that has broken off somewhere else in the circulatory system. The severity of the heart attack depends on how much heart muscle is affected. The smaller the area affected, the greater the chance of recovery.
If the heart attack is severe, and a large part of the heart muscle is affected, the heart can experience ventricular fibrillation: instead of co-ordinated beating, the individual muscle fibres contract in an unsynchronised way. The affected part, usually the left ventricle, sometimes becomes unable to pump blood and the heart stops. People who have had severe heart attacks can be resuscitated using electric shocks delivered to the chest; this restarts the heart and enables it to re-establish a normal beating rhythm.
Heart failure
The term heart failure suggests a condition in which the heart suddenly comes to a complete stop. This doesn't happen - heart failure usually develops slowly, often over years, as the heart gradually loses its pumping ability and works less efficiently. The underlying cause is usually coronary artery disease.
How serious the condition is depends on how much pumping capacity the heart has lost. Nearly everyone loses some pumping capacity as they get older but the loss is significantly more in heart failure.
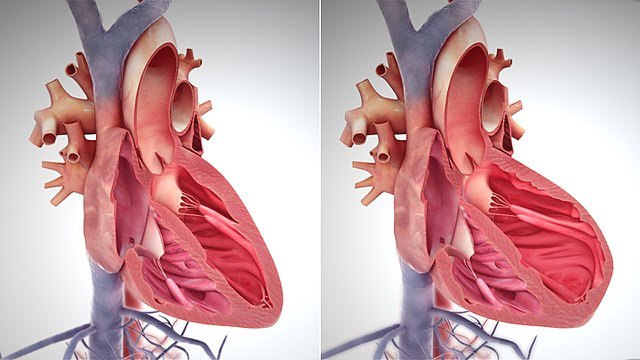
There are two main types of heart failure:
Systolic heart failure occurs when the heart's ability
to contract decreases. The heart cannot pump with the force required to push enough blood out through the aorta. Blood coming into the heart from the lungs can back up and cause fluid to leak into the lungs, a condition known as pulmonary congestion.Diastolic heart failure occurs when the heart has a problem relaxing. The heart can't fill with blood because the muscles of the atria and ventricles have become stiff. People with this form of heart failure accumulate fluid, especially in the legs, ankles and feet. Their condition is called oedema.
Tiredness, breathlessness and excess fluid retention are common symptoms but because heart failure usually develops slowly, these obvious signs often don't appear until the damage to the heart is serious. This is partly because the heart adjusts to cope with the effects of heart failure by getting bigger, developing thicker muscle and by contracting more often.
Heart failure is treated by a combination of lifestyle changes and drug treatment. Patients are advised to stop smoking, lose weight if necessary, avoid drinking alcohol, and change their diet to reduce the amount of salt and fat they eat. Regular, moderate exercise is also helpful, but this needs to be done only with a doctor's approval.
However, heart failure is always a serious condition because it poses an increased risk of sudden death, through cardiac arrest. Drugs are usually used to control the symptoms and to try to prevent them getting worse.
- Diuretics help reduce the amount of fluid in the body and are useful for patients with fluid retention and high blood pressure.
- The drug digitalis increases the force of the hearts contractions, helping to improve circulation.
- Recent studies have shown that drugs known as angiotensin-converting enzyme (ACE) inhibitors can be useful. ACE inhibitors improve survival among heart failure patients and can slow, or perhaps even prevent, the loss of heart-pumping activity.
Stroke
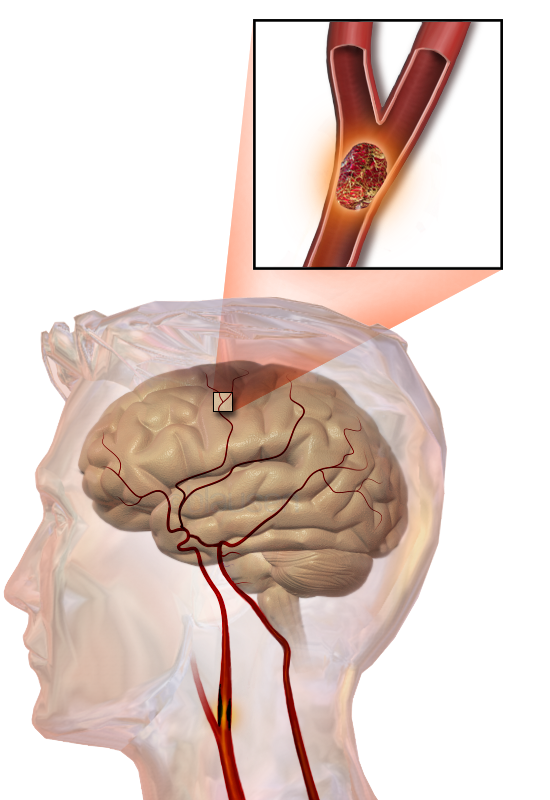
A stroke, or cerebral haemorrhage, results if the supply of blood to the brain is interrupted. The symptoms vary according to the size and location of the area affected. There might be no more than a tingling sensation or weakness down one side of the body, but at its most severe, a stroke can lead to permanent paralysis or death.
A stroke has several possible causes. One of the arteries in the brain could have developed an atheroma that has blocked the vessel, cutting of the blood supply to part of the brain. Or a clot that developed elsewhere in the body could have travelled through the carotid artery and then lodged in a smaller artery, with the same result. More rarely, an atheroma can lead to an aneurysm that ruptures causing blood loss and damage to brain tissue.
Angina
Angina pectoris is a severe pain in the chest that occurs when the coronary arteries are unable to supply sufficient oxygen to the heart muscles.
Angina is often the result of an atheroma in the coronary arteries. As the arteries become narrower, the supply of oxygenated blood to the heart muscle becomes more erratic.
Thrombophlebitis
Thrombophlebitis occurs when a vein is damaged and develops a blood clot that blocks it. Blood clots in the leg veins can occur in patients who are forced to remain in bed for long periods.
A thrombosis is the blockage of an artery caused by a blood clot. It can occur anywhere in the body. An embolism occurs when a mobile blood clot (called an embolus, hence embolism) moves through the circulatory system and then lodges in a vein and blocks it. If a pulmonary vein (from lungs to heart) becomes blocked, this causes a pulmonary embolism that can be fatal.
A blood clot or thrombus can form when a tibrous atheroma plague bursts into an artery. This caption points to the main femoral artery, but a thrombus can occur anywhere in the body. The cells underneath the endothelium are exposed to the blood and trigger the blood clotting mechanism.
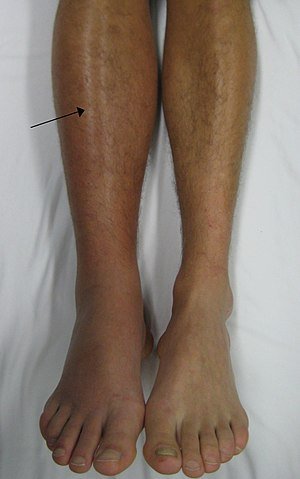
A thrombus forms, and if this breaks free and lodge in one of the arteries supplying the heart, it can cause a heart attack. If it lodges in one of the arteries that leads to the brain this can obstruct blood flow and result in a stroke.
Aneurysm
An aneurysm results from a tear in the wall of an artery. This allows blood to enter the muscle layer of the artery and produce a balloon-like swelling. If this swelling bursts, the consequences are usually fatal. An aneurysm can also occur in the wall of the left ventricle after a heart attack.
THE LINK BETWEEN ATHEROSCLEROSIS AND CARDIOVASCULAR DISEASE
To understand how and why cardiovascular disease develops, we need to look
at three things:
- How does an atheroma form?
- How does atherosclerosis lead to cardiovascular disease?
- What are the risk factors associated with atherosclerosis and how do they increase the chance of atheroma formation?
The formation of an atheroma
Atheromas, areas or plaques of fatty material, develop on the inside of arterial walls. Remind yourself of the structure of an artery wall by looking at the diagram below. As plaques build up, they can affect the circulatory system by:
- Blocking the flow of blood through the artery.
- Initiating the formation of blood clots. Blood clots that form inside coronary arteries are particularly dangerous. They can break free and lodge in the smaller coronary arteries, causing some of the heart muscle to die. This is what initiates a heart attack. If blood clots interfere with the blood supply to the brain, the result is a stroke.
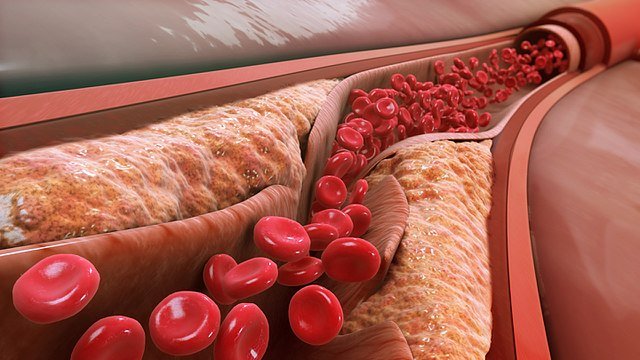
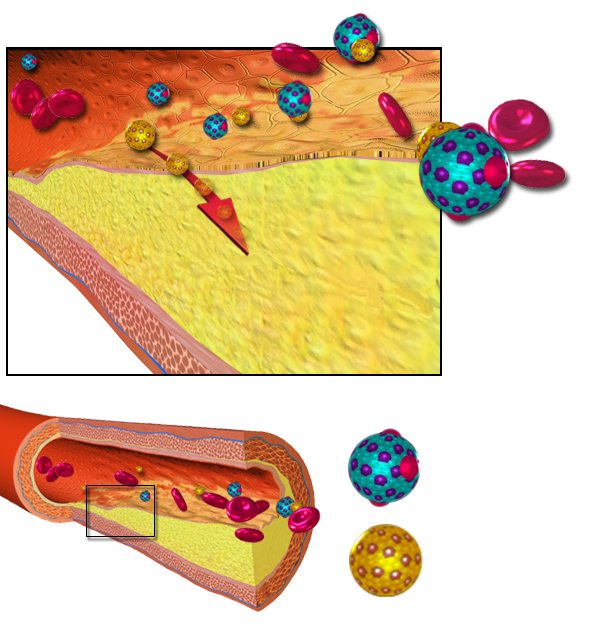
Arterial blood supplies all the body's organs with nutrients, including triglycerides and cholesterol. These are lipids and have several important functions in the body: they form cell membranes and they act as energy sttores. Lipids combine with proteins to form lipoproteins before they can be transported in the blood.
Lipoproteins that contain cholesterol are engulfed by white cells called phagocytes that occur in the artery wall, just under the endothelium. If the blood contains large amounts of cholesterol-rich lipoproteins, large numbers of stuffed phagocytes accumulate. Their rich 'filling' gives them a foamy appearance and they are, in fact, often referred to as foam cells.
When patches or streaks of foam cells start to appear on the inside of artery walls, this is recognised as the first sign of atherosclerosis. At this stage, there is little effect on the flow of blood through the artery and no discernible symptoms.
HOW DOES ATHEROMA LEAD TO CARDIOVASCULAR DISEASE?
Gradually, usually over many years, muscle cells and fibres begin to grow over the affected patches, giving rise to a fibrous plaque. This bulges into the lumen of the artery and starts to obstruct the flow of blood. This can have one of several effects:
- The artery can become very narrow. Depending on the position of the narrowed artery, the oxygen supply to vital parts of the body can be reduced. If, for example, the arteries feeding the heart muscle are affected, the result can be angina.
- The blood vessel can become completely blocked. Blockage of an artery that takes oxygenated blood to a vital organ can lead to many different problems. If the coronary arteries become blocked, the result can be a heart attack, If arteries in the brain are affected, this can lead to a stroke.
- The blood vessel can burst. A burst artery, or aneurysm, inside the body is very serious. If one of the main arteries near the heart burst, this is usually fatal.
- A The plaque can burst into the blood vessel, damaging the endothelium. When the cells underneath come into contact with blood, this triggers the blood-clotting mechanism. A blood clot or thrombus forms in the vessel. If this breaks free, it can travel around the body and block an artery or a vein, causing an embolism or a thrombus.
RISK FACTORS ASSOCIATED WITH ATHEROSCLEROSIS AND CARDIOVASCULAR DISEASE
As you have seen, the underlying process of atherosclerosis can have many different effects, depending on which part of the body is involved. The risk factors for cardiovascular diseases (CVDs) are also complex because many different factors affect the way this whole body system functions. I shall look at the three main ones that have been identified.
Hypertension
Blood vessels are more than a series of pipes that take blood to and from different organs. They react to the changing needs of the body supplying, for example, more blood to the muscles during exercise. When we make our muscles work hard, they need more oxygen and more glucose and they also produce more carbon dioxide. So, the supply of blood to different organs changes as we do different activities.
Think about an exercising muscle. How can it get more blood? Although blood vessels are flexible, they don't just expand and let more blood through. If this were to happen, the blood would just flow more slowly and no extra oxygen would actually reach the muscle. An increase in blood pressure is heeded. This speeds up the blood flow so that more blood reaches the muscle in a given time, supplying more oxygen and glucose to muscle cells and removing waste products more rapidly. Contraction of the smooth muscle in the walls of the body's arteries helps to bring about this increase in pressure.
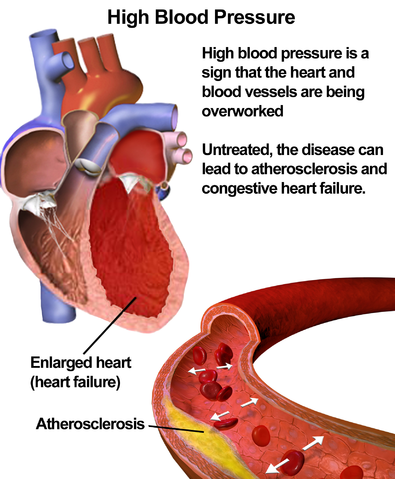
High blood pressure is perfectly normal as long as it results from short-term fluctuations in blood flow. Problems start when the blood pressure stays higher than normal while someone is at rest. This person is suffering from high blood pressure, or hypertension.
Hypertension sets up a sequence of events that becomes a vicious circle. Smooth muscle in the artery walls responds to an increase in blood pressure in the same way that skeletal muscle responds to extra exercise - it increases in size. This results in a thickening of the artery wall and a narrowing of the lumen. The volume of blood passing through the arteries remains the same, causing the blood pressure to rise further. At higher pressure, the blood also exerts a greater force on the endothelial cells that line artery and these cells are more likely to become damaged. Small flaws in the lining of the artery increase the risk that an atheroma will form. This, in turn, makes it more likely that a thrombosis will develop.
Two things increase the risk of hypertension. A high salt intake is one, If you increase the salt concentration of your blood, its water potential falls. A lower water potential means that blood volume increases as water is drawn from the cells of the body into the plasma. The higher the volume of the blood, the greater its pressure. The other is smoking.
To avoid a too lengthy post, I'll stop here for now. In my next post, I will explain the link between smoking and diet with atherosclerosis, treating of cardiovascular diseases and how to prevent them.
Thank you for reading
REFERENCES
https://www.medicalnewstoday.com/articles/237191
https://www.medicalnewstoday.com/articles/257484
https://www.webmd.com/heart-disease/guide/diseases-cardiovascular
https://www.webmd.com/heart-disease/guide/heart-disease-heart-attacks
https://en.wikipedia.org/wiki/Heart_failure
https://emedicine.medscape.com/article/163062-overview
https://www.mayoclinic.org/diseases-conditions/heart-failure/symptoms-causes/syc-20373142
https://en.wikipedia.org/wiki/Stroke
https://www.medicalnewstoday.com/articles/7624
https://www.mayoclinic.org/diseases-conditions/stroke/symptoms-causes/syc-20350113
https://www.nhs.uk/conditions/angina/
https://www.heart.org/en/health-topics/heart-attack/angina-chest-pain
https://en.wikipedia.org/wiki/Thrombophlebitis
https://www.mayoclinic.org/diseases-conditions/thrombophlebitis/symptoms-causes/syc-20354607
https://www.mayoclinic.org/diseases-conditions/brain-aneurysm/symptoms-causes/syc-20361483
https://www.medicalnewstoday.com/articles/156993
https://www.ncbi.nlm.nih.gov/books/NBK218744/
https://www.webmd.com/heart-disease/atherosclerosis-and-coronary-artery-disease
https://en.wikipedia.org/wiki/Atheroma
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3658954/
https://www.webmd.com/heart-disease/what-is-atherosclerosis
https://www.nhlbi.nih.gov/health-topics/atherosclerosis
https://www.ahajournals.org/doi/abs/10.1161/01.cir.0000131513.33892.5b
https://www.ncbi.nlm.nih.gov/pubmed/3772910
https://en.wikipedia.org/wiki/Hypertension
https://www.who.int/news-room/fact-sheets/detail/hypertension
https://www.medicalnewstoday.com/articles/150109
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider supporting our funding proposal, approving our witness (@stem.witness) or delegating to the @steemstem account (for some ROI).
Please consider using the STEMsocial app app and including @stemsocial as a beneficiary to get a stronger support.
Congratulations @loveforlove! You have completed the following achievement on the Hive blockchain and have been rewarded with new badge(s) :
You can view your badges on your board and compare to others on the Ranking
If you no longer want to receive notifications, reply to this comment with the word
STOPDo not miss the last post from @hivebuzz: