Electrical Conduction System of the Heart
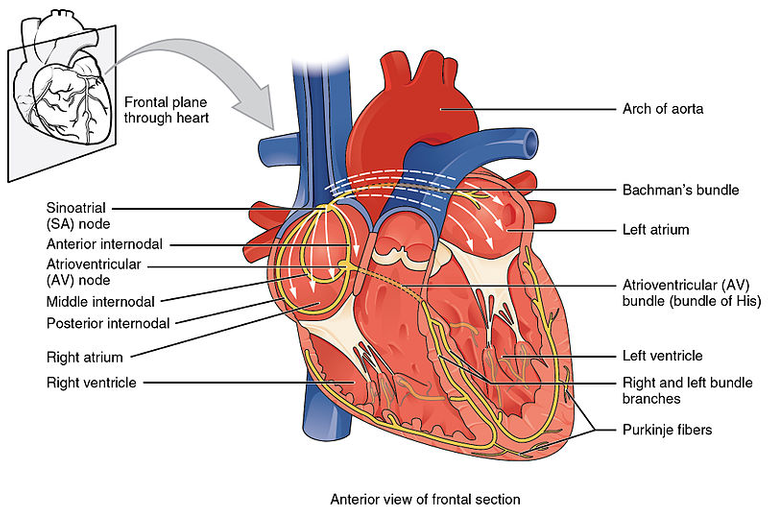
Picture from Wikipedia
Introduction
The myocardium is made up of three different kinds of cells: the cells that make up the pacemaker, the cells that send electrical signals, and the myocardial cells. Pacemaker cells, or nodal cells, are the cells that are in the sinoatrial (SA) and atrioventricular (AV) nodes. Action potentials, which are also called electrical impulses, are made when these cells depolarize on their own. Action potentials send the signal for the atrium and ventricles to contract. Specialized conducting cells send action potentials quickly from the SA to the AV node and then from the AV node to the rest of the ventricular cells.
Some of these highly specialized conducting cells are named after the scientists who first figured out what they did. For example, once action potentials pass through the septum in the proximal part of the AV node, they go into the Bundle of His and quickly move through the Purkinje fibers, which end in the ventricles. This process keeps going until the action potentials get to the ventricles, where they belong. Conducting cells are needed because they are in charge of sending the electrical signal to all of the ventricles. This is a key step in making sure that the contractions happen at the right time.
Depolarizing the pacemaker
The pacemaker cells in the nodes can drop their voltage on their own until they reach their threshold number. In this way, they can make action potentials even if they don't have neurons, hormones, or cells that are close to each other. Each action potential they make makes the heart tighten as it moves through the body. Most of the time, the SA node controls how fast the heart beats. This is called "overdrive suppression." This is because the SA node loses its electrical charge more quickly than the AV node.
Once the trigger voltage is met, the action potential will start to spread. The opening of voltage-gated sodium channels causes the fast depolarization that happens at the start of the action potential in skeletal muscle cells and neurons. But these channels do not open in the cells that make up the heart's pacemaker, so this fast depolarization does not happen. Instead, L-type calcium channels open, which lets calcium rush into the cells and cause an upstroke. One of the biggest differences between skeletal or nervous system cells and heart cells is that an action potential is not caused by sodium but by calcium from the outside.
The myocardial cell is the heart's third variety of cardiac cells. Cardiac muscle fibers are responsible for nearly all of the heart's mass. Most of the heart's mass and the result of the heart's contractions circulate blood. Myocardial cells are responsible for the heart's steady rhythm, which is necessary for the circulation of blood throughout the body. These cells have evolved to the point where they can generate and transmit electric current. This allows the cardiac muscle to regulate its contraction and relaxation. Squeezing would be impossible without these cells.
The heart's intercalated discs are the structures responsible for connecting the cardiac muscle to its nerves. When these plates compress, they allow the heart's muscles to contract simultaneously, which is crucial for the organ to function properly. As a result of their gap junctions, ions can freely travel between cells. This facilitates the rapid transmission of electrical signals that regulate the heart's beating action. These signals regulate cardiac rate so that it is optimal for the body. The physical links between neighboring cells are these spheres. Gap junctions are a collection of proteins that connect cells in specific ways. Gap connections allow for the instantaneous transmission of electrical information. That's why the depolarization of one cardiac cell can spread to the rest of the heart in the long run. This demonstrates the cooperative nature of cardiac cells, which is essential for the heart's ability to contract and circulate blood efficiently as a whole. Thanks to gap junctions, ions like calcium can move rapidly and readily between heart cells. The heart has superior conduction of electricity compared to other organs because of the presence of intercalated disks and gap junctions. Because of this, the heart's action potential can rapidly propagate throughout the entire tissue.
The process by which the heart generates and transmits electrical signals
Being able to maintain a regular heartbeat without external stimulation is a part of it. This is made possible by specific heart cells' ability to initiate electrical impulses and propagate them throughout the entire heart. These impulses then trigger coordinated muscle contractions, which push blood throughout the body. But cardiac arrhythmias and other heart diseases can be brought on by issues with this mechanism. The sinoatrial (SA) node consists of a collection of specialized cells located in the top wall of the right atrium. These cells, when depolarized on their own, transmit a signal to the atrium and ventricle, which causes those chambers to contract. The SA node is sometimes referred to as the "pacemaker" of the heart because it constantly sends out this signal. The heart's action potentials keep it beating continuously. This is vital for the heart and the vascular system to function properly.
It is in the wall that separates the atria and ventricles that you'll find the atrioventricular (AV) node. The atrioventricular (AV) node is ready to take over for the sinus atrioventricular (SA) node if the SA node suddenly ceases regulating the heart's rhythm. Its cells can depolarize on their own, though much more slowly than the SA node. The SA node typically "wins" the speed competition because it generates action potentials at a quicker rate than the other nodes. We use the term "overdrive suppression" to describe this phenomenon.
This is why it is commonly believed that the heart possesses automaticity, the ability to pulse without conscious input. The heart is the "pump that never stops" because of this. The heart also has rhythmicity, meaning it can regulate its own pace of beating with each pulse. Even after being removed from the body, a healthy heart will continue to pulse if placed in an artificial energy source. The process of transporting tissues for transplant purposes involves this.
Spontaneous depolarization and the occurrence of action potentials
The heart's rate of natural depolarization (and thus, heart rate) is largely determined by the autonomic nervous system, but it can be altered by conscious control. The sympathetic and parasympathetic branches of the autonomic nervous system send nerve impulses to the SA and AV nodes. Consequently, the rate at which the nodes depolarize is altered. Accelerating heart rate is a result of the autonomic nervous system increasing the frequency with which the SA node depolarizes. The parasympathetic nervous system does the opposite of the sympathetic nervous system. The rate at which the heart beats is controlled more by the parasympathetic nervous system when the body is at rest. Without the parasympathetic nervous system's regulation, most individuals experience an increase of 100 bpm or so in heart rate. similar to how the pacemaker cells in the AV nerve depolarize on their own, but at a rate of about 50 heartbeats per minute.
Heart conduction and electrical action
The heart begins to pulse when cells in the SA node begin dissipating their electrical charge. An action potential is a specific type of electromotive force. The signal can propagate either from node to node along the conducting cells of the internodal conducting route or directly from cell to cell. The internodal conducting pathway is composed of three conducting cell paths that run in parallel and link SA and AV nodes. The Purkinje fibers carry the information from the AV node out of the brain via the bundle of His. Since the impulses originate in the atria, they can move rapidly through the ventricular heart.
It's not as simple as the internodal conducting cells relaying an action potential from one node to the next. In the atria and ventricles, they also travel straight from one cell to the next. The action potentials travel from one node to the next via the inter-nodal conducting cells, and this is done on top of that. Therefore, the cells surrounding the SA node also lose polarization when the cells inside the SA node do. The atria are made up of many different types of muscle cells, and an electrical signal must travel rapidly between them all. The contracting atria push blood into the heart's ventricles when all of the atrial muscle cells depolarize at the same moment. This therapy is essential to guarantee adequate blood supply to the heart and proper cardiac function.
References
- CCCOnline. n.d. Cardiovascular Levels of Organization – Anatomy & Physiology. Cardiovascular Levels of Organization – Anatomy & Physiology. https://pressbooks.ccconline.org/bio106/chapter/cardiovascular-levels-of-organization/.
- @ClevelandClinic. n.d. Heart Conduction: What Is It & How It Works. Cleveland Clinic. https://my.clevelandclinic.org/health/body/21648-heart-conduction-system.
- Anatomy and Function of the Heart’s Electrical System. 2021, August 8. Anatomy and Function of the Heart’s Electrical System | Johns Hopkins Medicine. https://www.hopkinsmedicine.org/health/conditions-and-diseases/anatomy-and-function-of-the-hearts-electrical-system.
- Cardiac conduction system - Wikipedia. 2013, October 1. Cardiac conduction system - Wikipedia. https://en.wikipedia.org/wiki/Cardiac_conduction_system.
- Electrical Conduction System of the Heart - an overview | ScienceDirect Topics. n.d. Electrical Conduction System of the Heart - an overview | ScienceDirect Topics. https://doi.org/10.1016/B0-12-369400-0/00193-9.


Thanks so much for letting us know the electrical conductivity of the heart.
Anytime buddy. I really appreciate your time
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider delegating to the @stemsocial account (85% of the curation rewards are returned).
Thanks for including @stemsocial as a beneficiary, which gives you stronger support.