Do you know about gangrene? Uncommon but deadly disease of today!!!

https://www.picpedia.org/medical-05/g/gangrene.html
Hello once again, it's time for another installment of my health care blog, and today I'll be discussing an illness that frequently manifests itself in people with diabetes and those who have sustained a long-term open wound. The lack of blood in the body's systems is the root cause of this ailment, yet it has far-reaching consequences. Let's get right to the point and reveal the article's topic.
To begin, what exactly is the condition known as gangrene? Gangrene is a condition that develops when an area of the body is deprived of its blood supply. This could be the result of a physical injury, an infectious disease, or something else else. This condition, which affects the lower extremities and can be brought on by a severe lack of blood supply or a significant bacterial infection, is referred to as gangrene. Toenails are the most likely to be affected by this condition, even more so than other areas of the body. People who have peripheral artery disease, which is a common circulation disorder in which restricted arteries limit blood flow to the limbs, have a higher risk of developing gangrene than people who do not have this condition.
Due to poor blood circulation and, in many cases, diminished sensation in the feet as a result of nerve loss, people with diabetes and peripheral artery disease are particularly susceptible to problems like gangrene. Toe tissue death can occur if an injured toe goes untreated for an extended period of time and if not enough blood is supplied to the area.
Discoloration, from very light purple to nearly black, is a common symptom of gangrene. There may be a distinct demarcation between the dead and living layers of skin. Infected areas of the skin often show signs of inflammation and may develop fluid-filled blisters. There is frequently a putrid odor.
Everyone, including men and women, are susceptible to getting gangrene. Diabetic and peripheral vascular disease patients frequently develop necrotizing fasciitis type I. In the general population, this is the most prevalent form of necrotizing fasciitis. The annual incidence of necrotizing fasciitis type II in the United States is between 5 and 10 per 100,000.. Half of the patients who get streptococcal necrotizing fasciitis are young and otherwise healthy.
Gas gangrene occurs at a rate of about 3,000 new cases per year in the United States Factors that typically predispose to this condition include severe penetrating trauma or crush injuries accompanied by cessation of blood flow. Clostridium septicum, the causative agent of spontaneous gas gangrene, may be more common than gangrene caused by other Clostridium species after trauma. C. perfringens, C. sordellii, and C. novyi are the most commonly implicated species in drug abuse.
A variety of gangrene subtypes have been described below!!
• Gas gangrene
Clostridium bacteria are the causative agents of gas gangrene. These bacteria induce an infection, which in turn causes the affected area to grow gas bubbles and poisons within it. The death of tissue is caused by the gases that are produced. This particular form of gangrene can be lethal, but it's quite uncommon.
• Dry gangrene
Your body cannot exist without oxygen reaching all of its cells and organs. You get oxygen from your lungs to the rest of your body via your blood. When an area of your body stops receiving adequate oxygen, dry gangrene develops. After some time, the affected body part will begin to degenerate and eventually perish. Skin closure and the absence of infection are hallmarks of dry gangrene.
• Wet gangrene
The condition known as "wet gangrene" occurs when germs invade and infect the body's tissues.
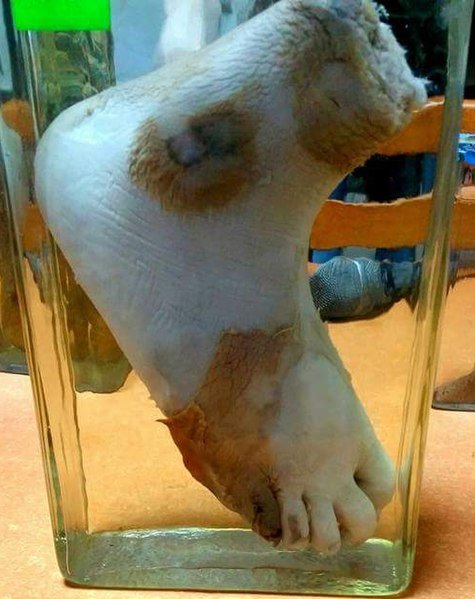
Wet gangrene of the foot
Wikipedia
Because of the bacteria, the tissues get swollen and eventually degrade. Your tissues will inevitably perish as a result of this procedure. There is a greater sense of urgency than in the case of dry gangrene due to the potential for systemic infection.
The presence of complications is contingent on the location of the gangrene within the body, the severity of the condition, the underlying cause of the gangrene, and the individual's general health. Some examples of complications are as follows:
Incapacity brought on by amputating limbs or removing dead tissue
Incomplete or sluggish wound healing, which may necessitate reconstructive surgery such as skin grafting;
To tell us how we can detect the existence of this illness, physicians may employ the following:
• Radiological examinations: X-rays, MRI, and CT scans are all useful for diagnosing gangrene and tracking its spread; additionally, they allow for the examination of blood arteries to spot any blockages.
When gangrene is suspected in a more internal organ, a surgeon may need to do an invasive, under-the-skin examination to confirm the diagnosis.
What hope do we have for curing this disease? After we have finished our testing, what options do we have?
Your treatment plan will be individualized based on your specific symptoms, age, and current health status. This will be determined in part by the severity of the ailment.
Antibiotics can be applied to the area to rid it of any lingering bacteria. Their sole application is in the treatment of wet gangrene.
We can use debridement which is refers to surgical removal of dead tissue when the area of death is localized, leaving healthy tissue unharmed. It can aid in preventing the gangrene from spreading to surrounding healthy tissues. If the gangrene has gone too far or is too far along the digit or limb, it may be necessary to amputate it.
In place of invasive surgery, you could try maggot debridement. Larvae of specific types of flies are applied to the injury. They eliminate microorganisms and chew away at decaying tissue. As far as medical procedures go, this one is completely painless.
Hyperbaric oxygen therapy involves being treated in a pressurized chamber that delivers oxygen at high pressures to increase the amount of oxygen reaching the affected area. Possible use in combating infection and speeding up the healing process by killing germs. Diabetic foot ulcers that progress to gangrene respond favorably to this treatment.
If your gangrene is the result of inadequate circulation, your doctor may propose vascular surgery to restore blood flow. If a clogged artery is to blame for a person's gangrene, for instance, the person may be a candidate for bypass surgery or angioplasty.
That brings us to the conclusion. I want to express my gratitude to you for taking the time to read this post, and I pray that God will richly reward you.

References
Buboltz, Jerome B., and Heather M. Murphy-Lavoie. “Gas Gangrene - StatPearls - NCBI Bookshelf.” Gas Gangrene - StatPearls - NCBI Bookshelf, www.ncbi.nlm.nih.gov, 10 May 2022, https://www.ncbi.nlm.nih.gov/books/NBK537030/.
Brusch, John L. “Gas Gangrene (Clostridial Myonecrosis): Background, Pathophysiology, Epidemiology.” Gas Gangrene (Clostridial Myonecrosis): Background, Pathophysiology, Epidemiology, emedicine.medscape.com, 13 Aug. 2019, https://emedicine.medscape.com/article/217943-overview.
Giri, Biplab, and Labanyamoy Kole. “Combating the Insidious Enemy: Epidemiology, Pathophysiology, and Treatment of Clostridial Gas Gangrene | SpringerLink.” Combating the Insidious Enemy: Epidemiology, Pathophysiology, and Treatment of Clostridial Gas Gangrene | SpringerLink, link.springer.com, 9 Feb. 2021, https://link.springer.com/referenceworkentry/10.1007/978-94-007-5869-8_36.
“Gas Gangrene - Microbewiki.” Gas Gangrene - Microbewiki, microbewiki.kenyon.edu, https://microbewiki.kenyon.edu/index.php/Gas_gangrene. Accessed 23 Aug. 2022.


Sounds like a lot of the usual #bigmed #massmurder jargon to hide truth so real healing methods do not come to light! in-courage you to dig deeper, beyond the lies for profit.
if you're open to this, to look beyond the programming of #thepowersthatshouldntbe, i'll be happy to point you in some good directions.
Sat Nam
Atma
!HBIT !LUV !PIZZA
@atma.love(2/3) gave you LUV. tools | wallet | discord | community | <>< daily
tools | wallet | discord | community | <>< daily
HiveBuzz.me NFT for Peace
Friend, I don't quite understand your comment.
PIZZA Holders sent $PIZZA tips in this post's comments:
atma.love tipped jsalvage (x1)
@curation-cartel(6/20) tipped @jsalvage (x1)
Join us in Discord!
Dear @jsalvage, Your article is good!
Thank you dear
I initially thought that gangrene is caused by deep wounds. I was once watching a WWII movie where the protagonist was wounded that he heat up his dagger and then pressed it against his wound. A war veteran by my side told me it was to prevent gangrene. That was the first time I heard about it.
Never knew a more about gangrene before your article.
I remember this kind of scene on an episode of a CSI that I watched a long time ago. I thought it can only happen as an accident and not possible to replicate it.
Thanks for sharing.
!1UP
You have received a 1UP from @thecuriousfool!
@stem-curator, @vyb-curator, @pob-curator, @neoxag-curator
And they will bring !PIZZA 🍕.
Learn more about our delegation service to earn daily rewards. Join the Cartel on Discord.
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider delegating to the @stemsocial account (85% of the curation rewards are returned).
You may also include @stemsocial as a beneficiary of the rewards of this post to get a stronger support.
This was a beautiful detailing on gangrene. In addition to the test done, Fasting plasma sugar can be tested to rule out the possible cause of nerve loss.
Thank you dear for your contribution. I believe that would be added into practice
This is actually the first time I am learning about this disease and I am really excited to learn about it from your blog, the good thing about steem social, is that there are always things to learn.
Yeah dear, this space literary provides us with many interesting articles daily. I love stemsocial too
Yeah I had a relative who had diabetes and she ignored the gangrene and they had to amputate her leg. She passed not long after that.
That's very bad. Sorry to hear about that. People should be concerned when experts tell them what to do when it comes to their health.