Antibiotic Resistance: An overview
Good health is essential, as the saying goes; health is wealth which is why people worldwide are quick to take medications to treat diseases. Drugs have physiological effects when ingested to help treat, cure or prevent diseases. They are also used to promote well-being. Sometimes, the overuse of certain medications like pain relief treatments may lead to addiction or drug resistance. I will focus on drug resistance in this article. Imagine being told that antibiotics cannot cure your urinary tract infection. It may sound unbelievable because you have effectively treated it in the past, but it can happen. Here's how:
Unlike treatable drug addiction, from repeated drug consumption, resistance is not a function of the body but instead of pathogens. Let me explain this. Drug resistance occurs when the pathogens in the body no longer respond to medications over time, so your body is not the one resisting the drug but the disease-causing organisms.
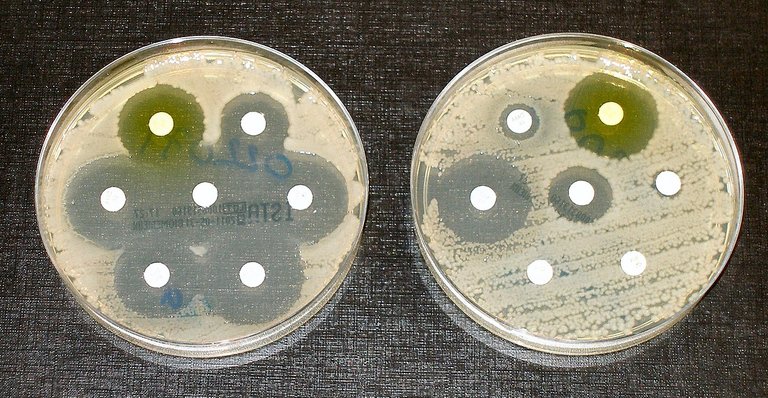
What causes drug resistance?
All over the world, antimicrobial drugs are often prescribed by doctors to treat infectious diseases from bacteria, parasites, fungi, and viruses. The frequent use of these drugs makes microbes adapt and grow resistant to them, making the drugs no longer potent in curing the diseases they cause. In many underdeveloped countries, these medications can be bought without a prescription; as such, people buy them without proper diagnosis whenever they feel symptoms of a previous disease that was treated by these antimicrobial drugs.
Another cause of drug resistance is when the patient does not finish the entire antimicrobial treatment. When drugs are not taken for the whole of the prescribed course, pathogenic bacteria can adapt to the presence of low dose since it is less harmful to them and eventually form a population that is entirely resistant to the antibiotic or antimicrobial drug regardless of the dosage.
The most common form of antimicrobial resistance is antibiotic resistance which is a result of its frequent use to treat some common diseases in plants and animals. Extensive use of these antibiotics in agriculture also poses a threat since these products are ingested by humans. Likewise, humans use antibiotics extensively to treat many diseases and prevent some. Some the diseases commonly treated by antibiotics in humans include:
Urinary tract infection:
This is an infection in any part of the urinary system, including the kidney, bladder, and urethra. It is a very common disease that affects about 1.5 million people yearly in Nigeria alone and is more common among women globally. Urinary tract infection is usually self-diagnosable, and when treated with antibiotics, it takes a few days or weeks to completely resolve.
Tetanus
This is a severe bacterial infection that is contracted when an opening in the body (wound) is exposed to the spores or any propagules of the bacterium, Clostridium tetani. Tetanus infection affects the nerves and causes muscle spasms; it can lead to death if not treated. The management of tetanus involves the use of antibiotics, but it can be prevented through vaccination.
Ear infection
A middle ear infection may be caused by bacteria, like Haemophilus influenzae and Streptococcus pneumonia, which are the two most common bacterial causes of ear infection, Viruses can also cause ear infections. Most ear infections result from other illnesses such as cold or flu, which cause congestion and inflammation of nasal passages. Antibiotics are usually prescribed to treat this infection.
Pneumonia
This infection arises when one or both air sacs in the lungs get inflamed and may be filled with fluid. The air sacs may fill with fluid or pus, and the infection can be life-threatening to anyone, particularly infants, children, and people over 65. It is not self-diagnosable; hence medical diagnosis through lab tests or imaging is always required. Symptoms of pneumonia include a cough with phlegm or pus, chills, difficulty breathing, and fever. Some types of pneumonia are preventable by vaccines, and treatment with antibiotics resolves the infection in a few days or weeks.
Why is antibiotic resistance a concern?
The rapid emergence of resistant bacteria worldwide has become a global crisis. Decades after antibiotics have successfully treated bacterial infection; it has once again become a threat. Alexander Fleming first discovered the era of modern antibiotics in 1928 with the discovery of penicillin. After which many antibiotics were developed, such as the beta-lactam antibiotics, which were developed when penicillin resistance was observed.
More than 150 million antibiotic prescriptions are written each year in the U.S. This frequent consumption has a major role in the development of antibiotic-resistant pathogens Antibacterial products sold for hygienic or cleaning purposes may also contribute to this problem. One disturbing fact about antibiotic resistance is that the pharmaceutical industry is developing very few new innovative antibiotics.
The medicines for chronic conditions are more profitable, in comparison to antibiotics which is why pharmaceutical companies prefer to invest in them. Some antibiotic-resistant bacterial infections are: Methicillin-resistant Staphylococcus, Aureus Vancomycin-resistant Enterococci, Drug-Resistant Streptococcus pneumonia among many other emerging antibiotic-resistant bacterial infections.
How to tackle antibiotic resistance
To help fight antibiotic resistance, the best thing to do is to avoid infections by protecting yourself against infectious diseases. Ensure your source of water is clean and maintain good hygiene. Please do not resort to antibiotics unless you are sure you need them by confirming from your doctor. Some common viral diseases like common cold, bronchitis, ear and sinus infections do not need antibiotics. You can also trust your immune system to fight some diseases by waiting it out if the symptoms are mild.
If antibiotics have been prescribed to you, take your entire prescription exactly as directed, even when you feel better before completing the drug course. When admitted to a hospital, ensure to stay safe, wash your hands regularly as the hospital houses many antibiotic-resistant bacteria. Prevent antibiotic infections by getting vaccinated to protect you against some diseases that are treated with antibiotics. These diseases include whooping cough and tetanus.
In conclusion, eating well is far better than any medicine that has been, and will ever be produced. There is a saying that if you do not make your food your medicine, you might end up making medicine your food. Eating well will shield you from many forms of diseases. Remember, prevention, they say, is better than cure.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5446555/
- https://www.cdc.gov/drugresistance/about.html
- https://www.who.int/news-room/fact-sheets/detail/antibiotic-resistance
- https://www.medicalnewstoday.com/articles/163063
- https://www.healthline.com/health/pneumonia
- https://my.clevelandclinic.org/health/diseases/9135-urinary-tract-infections
- https://www.medicalnewstoday.com/articles/167409
Your post has been voted as a part of Encouragement program. Keep up the good work!
Use Ecency daily to boost your growth on platform!
Support Ecency
Vote for Proposal
Delegate HP and earn more
I would say antibiotics leaking into the environment is probably the biggest contributor of drug resistance.
They pass through bodies, may that be humans or animals. Once the drugs are in the environment, they either kill off the susceptible bacteria or trigger their defense mechanisms. And here we are.
Rightly said. This is why there must be continued research into the development of novel drugs as well as how resistant development in microbes can be limited.
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider supporting our funding proposal, approving our witness (@stem.witness) or delegating to the @stemsocial account (for some ROI).
Please consider using the STEMsocial app app and including @stemsocial as a beneficiary to get a stronger support.