Neurology || Neuro Pathology of Epidural Hematoma
Over the last few days, we have been studying Neuro pathology, and I started with the Neuro Pathology of Spinal Cord Lesions, after which I wrote another post on the Neuro Pathology of Cerebral Palsy. You can take your time to read through these posts, and I am sure you would enjoy them. Still, on the Neuro Pathology series, I will be creating a post today on the pathology of Epidural Hematoma (EDH).
Introduction
Epidural Hematoma arises as a result of a bleed that accumulates within the epidural space. In simple terms, I will say it is a brain injury that occurs when a blood vessel in the skull ruptures allowing blood to accumulate in the dura mater thereby compressing and damaging the epidural space. In this post, I will be explaining the Anatomy of Skull meninges (Dura mater, Arachnoid mater, and Pia Mater), the Epidemiology of Epidural Hematoma, Etiology and Pathophysiology, CLinical features, Diagnosis, and Treatment.
Anatomy of the Cranial Meninges
I will be starting with the anatomy of the Skull meninges. The meninges is located between the brain parenchyma, and the skull. To explain clearly, the skull bone is the bone that is visible to the eyes. Below the bone is the Periosteal layer of the dura mater, followed by the meningeal layer of the dura mater. Between the meningeal layer and the periosteal layer is the epidural space where blood accumulates. The Arachnoid matter follows the meningeal layer, which is divided by the subdural space. Below the Arachnoid mater is Pia matter which clings to the brain parenchyma. Between the bone and the periosteal layer are blood vessels, one is known as the Middle meningeal artery, and another is known as the Anterior Ethmoidal Artery. If the middle meningeal artery is damaged, causing blood to leak into the periosteal dura mater, and the meningeal dura mater, it will lead to Epidural Hematoma.,,,.
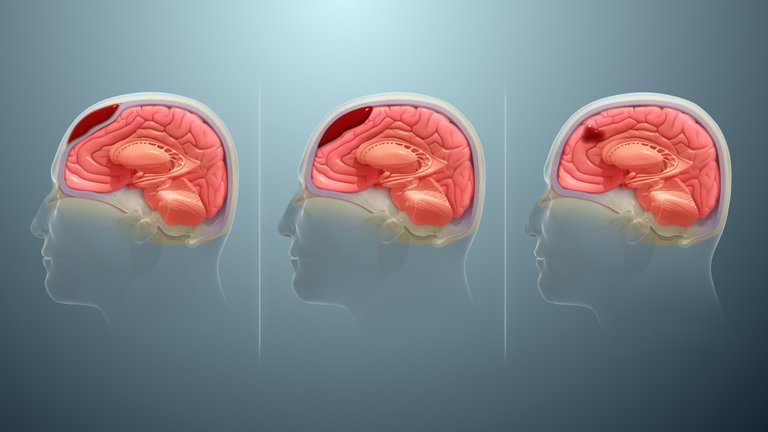
Epidermiology of Epidural Hematoma
Epidural Hematoma occurs in about 2% of head injuries, with about 75% of all adult cases affecting the temporal area of the brain. It makes up about 15% of all fetal head traumas affecting people adults, basically between the age of 20 to 30 years, and can also affect people above 50 years old, but this is a rare case. ,
Etiology and Pathophysiology of Epidural Hematoma
While I have discussed the anatomy of the meninges, and its epidemiology, I will be discussing its etiology and pathophysiology. Epidural Hematoma, can either be Arterial E.D.H., or Venous E.D.H. Arterial Epidural Hematoma is more common than Venous Epidural Hematoma.
Arterial Epidural Hematoma occurs as a result of the laceration of the middle meningeal artery which is common in the terion. Also, skull base fracture can lead to the laceration of the middle meningeal artery, as it enters through the foramen spinosum, Fracture from frontal bone injury can also lead to injury of the Anterior ethmoidal artery.,,,,
Venous Epidural Hematoma occurs as a result of injuries to the venous sinuses. These epidural hematomas can occur in places like the Superior Sagittal Sinus where there is a laceration around the vertex, it can also occur at the middle cranial fossa due to the Spheno parietal sinus producing epidural hematoma. Also, there can be an Epidural Hematoma as a result of a bleed from the transverse sinuses and sigmoid sinuses, causing Epidural Hematoma at the posterior cranial fossa.,,.
Traumas are usually the major causes of Epidural Hematoma, especially Arterial epidural hematoma. There can also be cases where it can occur not as a result of trauma. It can be a result of an infection such as in diseases like Otitis media, or Mastoiditis where the infection spread from the bone to the blood vessel thereby damaging it.,. Anticoagulant can also lead to Epidural Hematoma. When patients have coagulopathy such as when they have low platelet (thrombocytopenia and are on anticoagulants medication, and anti-platelets, there could be a case of Epidural Hematoma when the blood in the vessels cannot coagulate after a minor tear in the vessel. Where there is no functional coagulation system to plug up the tears, it will lead to bleeding causing Epidural Hematoma.. Another case that could lead to epidural hematoma is as a result of Arterio Venous Malformation where there isn't a through capillary causing pressure in the venous area, causing rupture which will lead to blood flowing into the Epidural space leading to Epidural Hematoma.. Cancers can also spread around the body, reaching the dura mater causing vascularity which could lead to bleeding around the dura mater.,.
If a person has an epidural hematoma in the coronal section, it would cause compression to the core of the brain, leading to issues such as the focal deficit, Herniation syndrome. People with epidural hematoma usually have a loss of consciousness due to concussion, they also would present with lucid intervals as a result of body shunting venous blood of the brain and less blood in the skull. Patients start to experience clinical deterioration when they experience herniation syndrome. ,
Clinical Features and Diagnosis and Treatment of Epidural Hematoma
The common symptom of Epidural Hematoma is headache, they may also experience loss of consciousness, clinical deterioration, and lucid intervals. When they start to show signs of Herniation syndrome, then it needs interventions. When there is pressure as a result of blood flow into the tissue of the brain, pushing the tissue underneath the Falx cerebri, it presents with subfalcine herniation, leading to Anterior cerebral artery syndrome, causing lower extremity weakness, and loss of senses in the lower extremities. ,. In cases of bilateral epidural bleeds, pushing the diencephalon pass the tentorium cerebelli, into the brain stem area causing stress to the basilar artery, causing Duret hemorrhages preventing the pupils to be dilated causing small and fixed pupils.,,,.
Diagnosis includes a Lab tests which includes checking the COAGS of the patients including the PT/INR, and PTT, CBC test can be done to check platelets to be sure if the patient has Thrombocytopenia, and check if patients are taking anticoagulant and anti-platelet. CT scan of the head will be done, looking at the bleed which will take a bi-concave or lens shape to bleed in the brain which does not cross the suture line, and the bleed is hyperdense. Windowing of the images can is done to confirm that there are no fractures of the bone of the skull, MRI Scan, and Angiography..
Treatment of Epidural hematoma can start with reversing coagulopathy, if the patient is having a Coagulopathy type of hematoma. In cases where the patient has low platelet, transfusion can be done to increase it. Surgical intervention is an option for correcting with the operation. Creating a Borr hole, performing a craniectomy, and removing the blood from the space.,
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider delegating to the @stemsocial account (85% of the curation rewards are returned).
Thanks for including @stemsocial as a beneficiary, which gives you stronger support.