Systemic lupus Erythematosus
Overview
SLE is a chronic autoimmune disorder in which the immune system attacks tissues of the body causing inflammation of connective tissues in every organ of the body.
The immune system is meant to fight infection in the body, however, this disease attacks healthy tissues of the body.
SLE is the most common and most severe type of lupus erythematosus. Lupus erythematosus is a collection of autoimmune diseases. Other types of lupus include cutaneous lupus, drug-induced lupus, and neonatal lupus.
SLE is a type of connective tissue disease characterized by multisystem inflammation with the generation of autoantibodies. Connective tissue diseases are diseases that affect the parts of the body that connect the structures of the body.
SLE is a rare multi-organ disease that can affect the brain, skin, joints, lungs, kidneys, and blood vessels. 90% of patients with this disease are females. The peak age of onset is between 20 and 30 years.
One thing that is important to note is; that autoimmune diseases are way commoner in females than in males.
What are the causes of SLE?
SLE has an unclear cause. There are, however, risk factors that put persons at risk for SLE.
• According to studies, 90 percent of women diagnosed with SLE are between the ages of 15 and 44 years old. This is the time when estrogen levels are at their peak. Women are more likely than men to acquire SLE as a result of hormonal changes. The use of estrogen in postmenopausal women raises the risk as well.
• The importance of genetic predisposition cannot be overstated. When compared to the overall population, there is a 29-fold increase in sibling risk. If one of the identical twins (monozygotic twins) is affected, there is a 24% chance that the other will be as well. With a concordance rate of 2 to 5%, this is less frequent in dizygotic twins (i.e. fraternal twins).
• In people who are sun-sensitive, exposure to the sun can cause skin sores. This is due to the fact that photosensitivity is a precursor to skin illness.
• Cigarette smoking and silica dust also increase the risk.
• Exposure to agricultural pesticides is also a risk factor.
• Vitamin D deficiency is a risk as well.
• SLE can also be triggered by medications such as anti-seizure drugs, anti-hypertensive drugs, and antibiotics. This is common among patients with drug-induced SLE and these patients usually feel better when they discontinue these medications.
• SLE is common among African Americans, Hispanics, and Asian Americans.
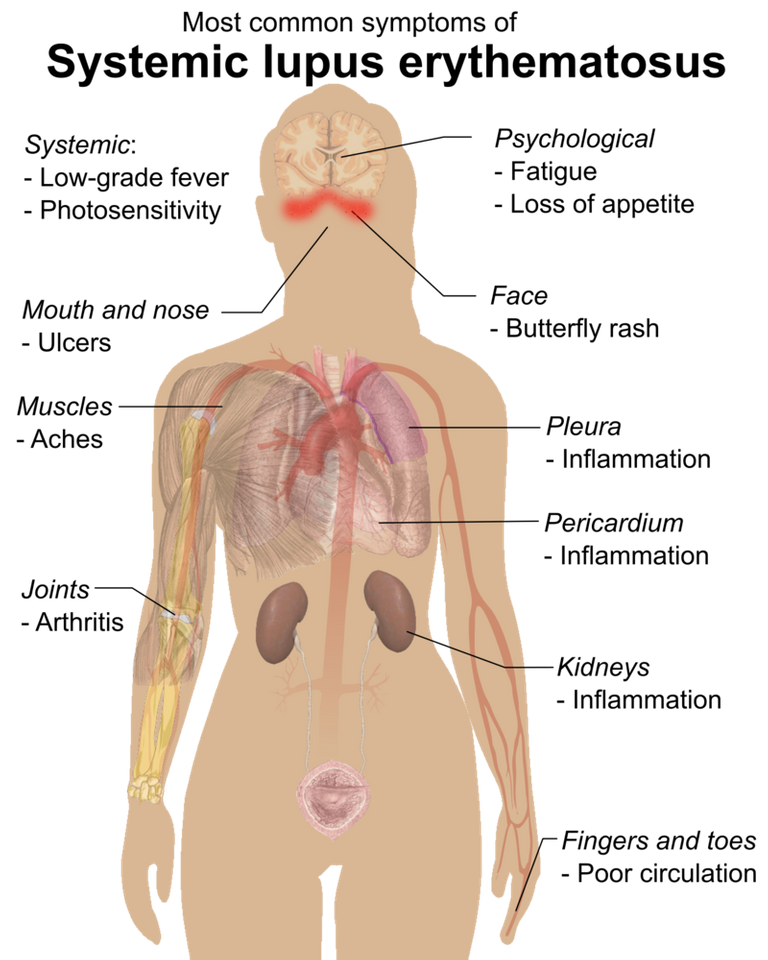
What are the signs and symptoms of SLE?
Häggström, Mikael (2014). "Medical gallery of Mikael Häggström 2014". WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.008. ISSN 2002-4436. Public Domain.orBy Mikael Häggström, used with permission. - All used images are in public domain., Public Domain, WikimediA
Because SLE has a tendency to look like other diseases, it is commonly misdiagnosed. The brain, heart, skin, kidneys, lungs, and muscles are among the organs affected by the signs and symptoms of a multi-organ disease. The following are some of the most common signs and symptoms of SLE:
• Malar rash i.e. a butterfly-shaped rash on the face that covers the cheeks and the bridge of the nose or rashes elsewhere on the body.

By Eva Rinaldi - Seal, CC BY-SA 2.0, Wikimedia
A picture of the popular musician with a lupus rash on the face
• Fatigue
• Fever
• Skin lesions that appear or worsen with exposure to sunlight
• Joint Pain
• Muscle Pain
• Chest Pain
• Malaise - feeling of unwell.
• Seizures, Confusion, Depression
• Weight changes
• Hair loss
• Raynaud’s Phenomenon i.e. fingers turning white or blue when cold

By Profpedia at English Wikipedia, CC BY-SA 4.0, Wikimedia
• Lymph node swelling
• Neutropenia, low neutrophil count, Thrombocytopenia, low platelet count. They might present with
How is SLE diagnosed?
It's worth noting that a triad of fever, joint pain, and rash in a woman of reproductive age could indicate SLE. This is a red flag that needs to be investigated further. A combination of clinical symptoms and test abnormalities are used to diagnose SLE.
The American College of Rheumatology (ACR) has suggested 11 classification criteria for SLE. Patients are considered to have SLE if they meet four of the following criteria:
• Malar rash
• Discoid rash
• Photosensitive rash
• Oral ulcers
• Nonerosive arthritis in 2 or more joints
• Pleuritis or pericarditis
• Glomerulonephritis or proteinuria
• Seizures or psychosis
• Hemolytic anemia, leukopenia, lymphopenia, or thrombocytopenia
• Immunologic laboratory abnormalities, such as antibodies to double-stranded DNA or the SM antigen or a false-positive serologic test for syphilis
• Positive ANA test that is not caused by a medication
Other than the ACR criteria, people with SLE may also have:
• Fever (over 100 °F/ 37.7 °C)
• Extreme fatigue
• Hair loss
• Raynaud’s Phenomenon
What are the complications of SLE?
Complications of SLE depend on the system involved. These complications include:
• Joint deformities
• Kidney failure secondary to a condition known as lupus nephritis
• Pleural Effusion which usually presents with difficulty in breathing. Most time oxygen support is needed
• Pleurisy - a condition in which there is chest pain on breathing in.
• Pulmonary Hypertension and Heart Attack
• Cytopenia -which is a reduction in the blood cell lines.
How Can SLE be treated?
Now that we've learned about the clinical aspects of SLE and the diagnostic criteria for the disease, let's look at the best ways to treat SLE patients. SLE is a disease for which there is currently no cure. It isn't contagious, thus it can't be spread from one person to another via touch. When people die, it's mainly due to the severity of their symptoms and organ damage.
As a result, with proper care and lifestyle changes, patients with SLE can enjoy healthy lives. Because SLE affects multiple organs, it needs interdisciplinary treatment. As a result, the medical team that treats SLE patients typically includes a variety of specialists. These experts include a rheumatologist, neurologist, cardiologist, nephrologist, dermatologist, hematologist, infectious disease specialist, pulmonologist, gastroenterologist, and a high-risk obstetrician, due to the possibility of poor pregnancy outcomes in pregnant SLE patients.
The treatment is also determined by the patient's symptoms and the severity of the sickness. The goal of management is to keep symptoms under control while also preventing multi-organ damage. SLE can range from mild to severe.
Patients with SLE should avoid being exposed to the sun and should use sunscreen. Exercise can also help to alleviate joint and muscular discomfort. For SLE patients, avoiding stress and getting enough sleep are key lifestyle changes.
Analgesics, Non-Steroidal Anti-Inflammatory Drugs (NSAIDs), and hydroxychloroquine are used to treat mild to moderate illnesses with symptoms limited to the skin and joints.NSAIDs should be used with caution as they can worsen the pain in patients with peptic ulcer disease. Also, NSAIDs can contribute to kidney failure when abused. Corticosteroids are also used in combination with immunosuppressants such as methotrexate or azathioprine. High-dose corticosteroids and immunosuppressants are used to treat life-threatening illnesses.
Mycophenolate mofetil (MMF), belimumab, rituximab, and cyclophosphamide are some of the other medications used to treat SLE.
Conclusion:
Therefore, if you have any of the symptoms mentioned or you know anyone that has these symptoms, it is important to visit a rheumatologist so that proper management can be started. Remember that having SLE is not a death sentence if properly managed by capable hands.
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider delegating to the @stemsocial account (85% of the curation rewards are returned).
You may also include @stemsocial as a beneficiary of the rewards of this post to get a stronger support.
Thanks for this interesting blog! I didn't know about SLE at all. After reading this post, I was a bit shocked, because of the "no cure" part? That's somewhat annoying... Do we have clues or ideas to follow to develop a cure, or are we still totally in the dark here?
Cheers!
Congratulations @bhoa! You have completed the following achievement on the Hive blockchain and have been rewarded with new badge(s):
Your next target is to reach 38000 upvotes.
You can view your badges on your board and compare yourself to others in the Ranking
If you no longer want to receive notifications, reply to this comment with the word
STOPSupport the HiveBuzz project. Vote for our proposal!