My very sad experience of losing a 3 year old child to sickle cell
The children emergency ward is a place where patients with life-threatening conditions are being brought to.
When these patients are brought here, they are being stabilized and sent to the lying in ward where more stable patients are kept.
Out of all the patients I saw, I discovered that most of the patients were children with sickle cell crisis.
Other conditions that came include; cerebral malaria, meningitis, bronchopneumonia, asthma and gastroenteritis.
The saddest experience I have had since I started clinical medicine was losing a 3-year-old baby to a sickle cell crisis.
She came in unconscious.
When I got to her bed she was having very serious seizures and she looked like she was having spasms.
I was a bit confused, at first, I thought it was tetanus.
Then I asked my colleagues about her diagnosis and it was the usual, sickle cell crisis.
This time it was not just sickle cell crisis, it was complicated with suspected meningitis based on the presence of seizures and loss of consciousness.
what is meningitis?
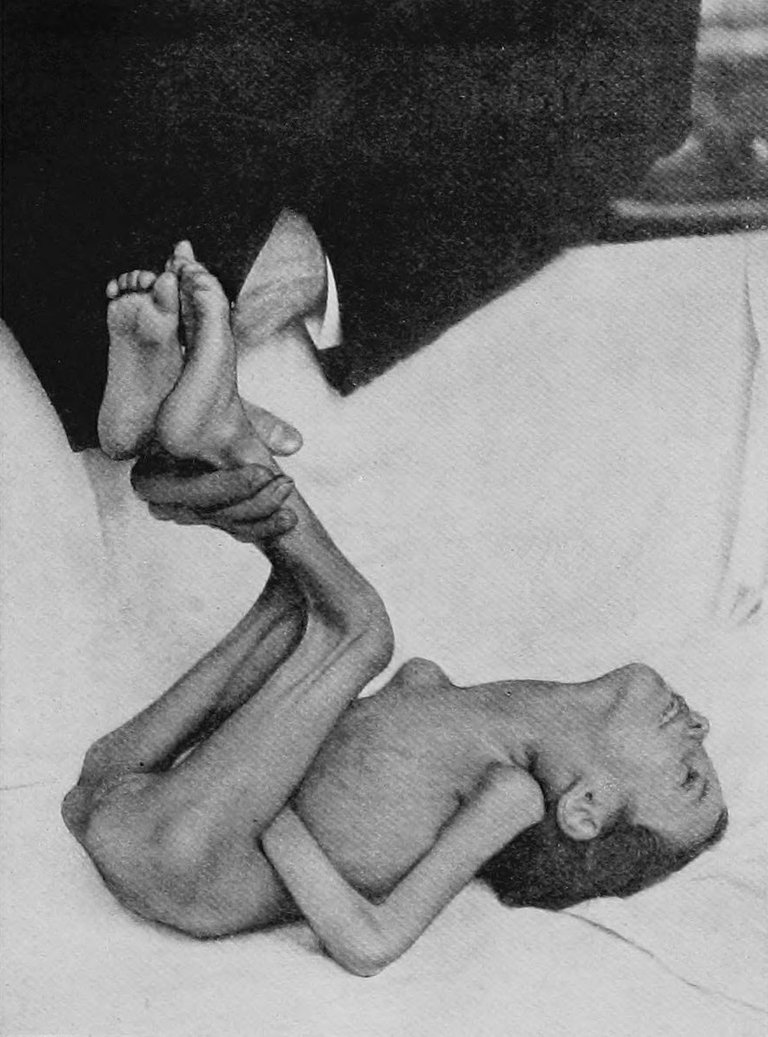
By R. G. Wiener, Harlem Hospital - Sahli, H. A treatise on diagnostic methods of examination (translation from the fourth revised & enlarged German edition). Saunders. 1909., Public Domain,Wikimedia
The meninges are the protective covering of the brain. They protect the brain.
The meninges are divided into three layers from outside to inside. The dura matter, the arachnoid matter and the pia matter.
When the meninges are inflamed, meningitis occurs.
Her Glasgow coma scale score at the time she was brought into the emergency was 6/15.
What is Glasgow Coma Scale?
Glasgow coma scale is a scale used to measure the level of consciousness a patient has.
When the score keeps reducing, it means the patient is getting worse and more importantly, there is a serious issue with the brain( more like the brain is getting dead)
After about 12 hours, the Glasgow coma scale score reduced to about 4/15.
Then I had to do her PCV, a test to check how much blood the child has in simple terms.
Her PCV was 20%. The normal for a healthy person is greater than 30% and it was 10% down.
So we had to transfuse her. Transfusion in paediatrics requires a lot of caution.
Transfusing a sickle cell patient must be with an AA blood.
She was a little 3-year-old girl who weighed 11kg.
So I had to transfuse her in aliquots so I don't get to overload her.
I had to use a 2ml syringe to give her 165mls of whole blood.
That means I was going to draw blood 82 times according to my registrar's plan.
I hate transfusing during night shifts but the baby was in dire need of blood.
I did the transfusion that night.
Before the transfusion, the Glasgow coma scale score was 4/15 b3fore the transfusion started.
I started transfusing by 9:55 pm and ended the transfusion by 11:10 pm.
I was tired and stained.
I cleared up the area and went to document everything that was done.
30 minutes later the baby started gasping.
At this point, Her GCS was 3, her heart was beating but she wasn't breathing.
A GCS of 3 means the child was brain dead.
Then I had to start resuscitating her. I had to use the bag and mask method.
I did this for like 2 hours.
My muscles were aching.
Then a few minutes later, there was no heart sound and my registrar stepped in and we started chest compressions.
Most times when chest compressions are initiated, we know the end is close.
I gave the first shot of adrenaline to see whether I could kick start the heart.
The heart didn't respond, I gave the second dose, the same thing.
Then I gave the last dose and continued compression.
Did the compression for about 30minutes and assessed the baby.
The pupils were not reactive.
There were no heart sounds.
The baby was cold.
She was certified dead at 3:20 am.
I was really really sad.
But why was I sad when I knew what the outcome was going to be?
I was sad because the mother had lost a child to a crisis too.
The second reason I was sad was that the husband never showed up.
She cried so bad that I felt it in my chest.
We decided to do a lumbar puncture to analyse the CSF and it was yellow and the CSF protein was greater than 100mg/dL.
The normal CSF is usually clear.
The whole brain was inflamed and the meninges were seriously affected.
She carried her baby alone to the mortuary.
So what was the point of these whole write up?
The first point is before getting married, do a genotype test.
Do it at least two times before getting married to that man or woman. In Nigeria, there are terrible labs and sometimes the result can be questionable.
So when doing a genotype test, do it in a standardized lab.Don't leave anything to chance. If your genotype is AS and your spouse is AS. You have two options if you stay in the tropics;
- Leave the relationship
- Get married and consider adoption.
Managing a sickle cell child is tasking. It requires motivation and commitment.
They are always on routine drugs that they are meant to take for a larger period of their life. They take malaria prophylaxis, bacteria infection prophylaxis, drugs for blood formation etc. If you don't have the strength to do this, then avoid the circumstance.
Children with sickle cell are prone to infections. These infections predispose and increase their chances of having a crisis or what is now called acute pain episodes.
An cute pain episode is something you don't want to see as a human being.
Out of the 15 patients I have managed, 12 of them came in crisis.
Lastly, if you have a child with - sickle cell, it is your duty to make the world a better place for them as this is not a death sentence and they are just as human as anyone.
If your genotype is SS, do well to get involved with someone who is AA.
Also, take your drugs well and drink a lot of water.
Thank you for reading.
!discovery 20
Thank you
This post was shared and voted inside the discord by the curators team of discovery-it
Join our community! hive-193212
Discovery-it is also a Witness, vote for us here
Delegate to us for passive income. Check our 80% fee-back Program
A really sad but relatable story. Are there things that could have been done better to save her life? Were you limited by available drugs, materials and equipment? The situation of the Nigerian health sector makes one to always ask this question each time an event like this occur.
Nevertheless, thanks for sharing your experience. It might be a sad one but it is insightful and educating.
BTW, it seems you forgot to include the source to the image used in your post.
Well, these are some of the problems of the health sector in Nigeria.
A lot of things could have been done. However, she didn't have funds and also the hospital was on strike.
She could have been put on a mechanical ventilator at least this would have taken care of her breathing.
She could also have been admitted into the intensive care unit. However, this requires a lot of money. The first day in the ICU costs about 50k.
My advice for everyone in this country is to try as much as possible to prevent every form of illness as this is not the best time to fall ill. Every doctor is leaving the country.
Mosquito nets for children
Healthy eating habits for everyone
Fruits and vegetables
Just prevention mainly. Nigeria is dying.
I am really sad sending this message
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider supporting our funding proposal, approving our witness (@stem.witness) or delegating to the @stemsocial account (for some ROI).
Please consider using the STEMsocial app app and including @stemsocial as a beneficiary to get a stronger support.
That's sad. I read yesterday there's a new treatment for sickle cell but there are no details yet.
Once you hear anything that ends with MAB... The cost is crazy.
They are antibodies.
In my opinion, no one should risk having a child with SS
Yeah money must be involved.
You know right