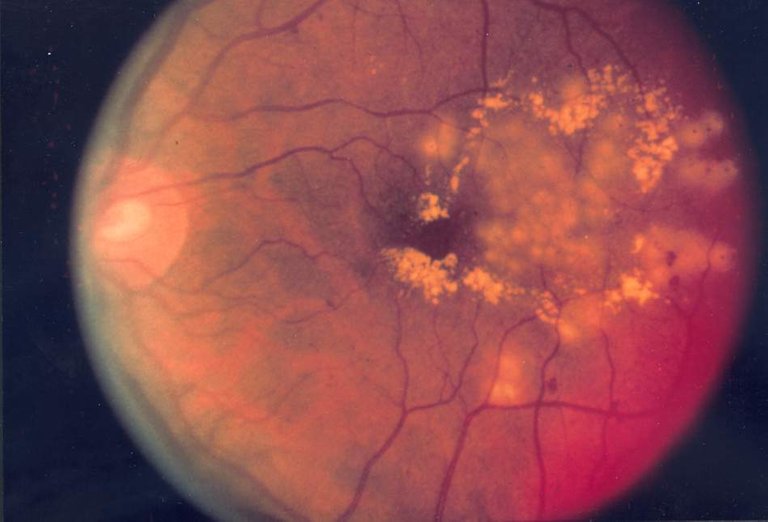
Blindness and diabetes(DIABETIC RETINOPATHY)
I noticed that majority of the patients were elderly people. What was most heart-breaking was realising that some of these patients were literally blind. Some could not read some letters on the Snellen chart, some could not count fingers just a few feet away from them, some could not see the movement of hands right in front of them and worse still, some could not even see light pointed right at them. What is more painful is that most people don't think of diabetes when they see a blind patient. They think of other things and forget to have a look at the blood glucose.
As I progressed in my Ophthalmology clinical posting, I learnt that there were a number of leading causes of blindness especially as a person advances in age and this includes cataract, glaucoma, corneal pathologies, age-related macular degeneration, diabetic retinopathy, hypertensive retinopathy and the likes.
In this article, the focus would be on diabetic retinopathy especially because diabetes is now a major public health issue worldwide with diabetic retinopathy, one of its complications. That said, with an increasing prevalence of diabetes across the general population, diabetic retinopathy may become one of the major leading causes of blindness worldwide. Hopefully, this could be averted with proper education of the masses.
What is diabetic retinopathy?
Diabetic retinopathy is a condition that occurs as a result of damage to the blood vessels of the retina in people who have diabetes. Diabetic retinopathy can develop if someone has either type 1 or 2 diabetes and a long history of uncontrolled high blood sugar levels. It is important to note that uncontrolled high blood sugar is the main problem. While one may start out with only mild vision problems, one can eventually lose sight.
Untreated diabetic retinopathy is one of the most common causes of blindness in the United States and in developed countries. It’s also the most common eye disease in people with diabetes.
There are different types of DR and this is based on their severity and if there is blood vessel affectation.
Nonproliferative diabetic retinopathy (NPDR): It’s called “nonproliferative” because the eye doesn’t make new blood vessels during the early stages. It has subtypes; background retinopathy and macula oedema. NPDR is commoner in patients who are newly diagnosed with DM as it doesn't usually present with symptoms.
During the early stages, damaged blood vessels often leak blood and fluid into the eye. However, in some cases, the centre of the retina (macula) is affected and it begins to swell. This condition is known as macula oedema and this is the subtype of non-proliferative DR that manifests with symptoms
Proliferative diabetic retinopathy (PDR): It is also called advanced retinopathy. It is the stage of retinopathy in which new blood vessels begin to grow within the retina in an attempt to replace the damaged vessels.
These new blood vessels are usually abnormal and grow in the centre of the eye and manifest with most of the symptoms people have.
What are the symptoms of DR
People with DR tend to have blurring of vision in the early stages than after a while shapes begin to float in their visual field or they begin to see dark spots.
It can get as worse as losing night vision and finally getting blind. Some studies have shown that some people present with difficulty distinguishing colours.
Aetiology:
When the level of sugar in the blood is high over a long period of time, diabetic retinopathy can occur following this. This excess sugar damages the blood vessels that supply the retina with blood.
The retina is a layer of tissue in the back of the eye. It’s responsible for changing images that the eye sees into nerve signals that the brain can understand. When blood vessels of the retina are damaged, they can become blocked which cuts off some of the retina’s blood supply. This loss of blood flow can cause other, weaker blood vessels to grow. These new blood vessels can leak and create scar tissue that can cause a loss of vision.
Risk factors:
The first and most important risk factor is poorly controlled diabetes. People with type 1 or type 2 diabetes are at risk for developing diabetic retinopathy.
Some studies have shown that Hispanics and African Americans are at a greater risk of developing diabetic retinopathy.
It has also been observed that people with other medical conditions such as high blood pressure and high cholesterol are at a greater risk of developing DR.
Pregnant women face a higher risk of developing diabetes and diabetic retinopathy. If a woman develops gestational diabetes, she has a higher risk of developing diabetes as she ages. The contention is which predisposes one more pregestational diabetes or gestational diabetes?
Finally, a positive family history of diabetic retinopathy increases the likelihood of developing diabetic retinopathy.

The original uploader was DyslexicEditor at English Wikipedia. - Originally from en.Wikipedia; description page is/was here., Public Domain, Wikimedia
The picture above shows normal vision. The picture below shows how a patient with diabetic retinopathy sees things
How to diagnose DR

By National Eye Institute, National Institutes of Health -(TIFF image), Public Domain, wikimedia
Most people with diabetic retinopathy tend to have complaints of blurry vision and other constitutional symptoms.
Some of them might even come or complain of things that are not related to the eye like recurrent infection, some might even come in with a foot ulcer, others might have CKD and this might just be the pointer to DR.
Sometimes, when people go to the hospital to complain of visual loss, sometimes they give them glasses thinking it's a refractive error. However, despite the change of glasses, there is still deterioration in vision, one should consider diabetic retinopathy.
By nei Public Domain, wikimedia
Another way of diagnosing DR is by evaluation of the ocular structures, including the evaluation of the retina through a dilated pupil with the aid of an ophthalmoscope or retinoscope, which is very helpful in diagnosing DR.
Treatment:
The treatment options for DR are limited. The ophthalmologist can perform regular eye exams to monitor the eye and check the progression of the disease.
An endocrinologist can help slow the progression of retinopathy by helping to optimally manage the blood sugar.
However, when it is advanced, the treatment options include;
Photocoagulation surgery (laser treatment): This surgery uses a laser to control or stop leakage by burning the vessels to seal them.
Vitrectomy is another procedure that involves removing scar tissue and cloudy fluid from the vitreous fluid of the eye. This procedure can also help alleviate the symptoms.
Some medications can be put in the eye to help reduce the formation of abnormal blood vessels. This, in turn, will help slow down the damaging effect of diabetic retinopathy.
They include Intravitreal injections of triamcinolone acetonide and anti-VEGF drugs such as bevacizumab.
Prevention
Prevention of diabetic retinopathy will always start with educating the public about diabetes and the eye. It also involves training doctors and other allied medical fields that deal with the eyes about diabetic retinopathy.
Another important way of preventing DR is by maintaining healthy levels of blood sugar and cholesterol.
Smoking has direct effects on blood vessels and for this reason, symptoms of diabetic retinopathy is worse in smokers.
The importance of exercise cannot be overemphasized as it helps with reducing blood glucose by pushing into the muscles.
Getting annual or 6-monthly eye checkups will go a long way in preventing and catching the disease early.
The takeaway:
Diabetic retinopathy is a serious eye condition that can lead to diminished eyesight or even blindness in those with diabetes. If someone has been diagnosed with diabetes, it’s important to do the following:
Get regular eye exams and physical checkups.
Keep the blood sugar, cholesterol and blood pressure at healthy levels.
Be mindful of any changes noticed in vision and discuss them with a doctor.
thanks for the enlightenment, this is also educating at the same time life saving. diabetes has been sickness that has no cure medically.
we have to be careful with are life, what we eat and how to live a healthy life, some people don't care about what they eat, they just consume whatever they feel like.
i think this article will help such person and save their life.
one more thing i will like to add is exercise, try as much as possible to exercise your body regularly, exercise don't allow some sickness in the body system.
The importance of exercise cannot be overemphasized when talking about diabetes. Diabetes is a global problem and we have to be careful in how we live our lives.
Thank you for stopping by
This is a good read and I agree a few things from it, especially having someone from the family having it. !discovery 18
Family history is one the not modifiable risk factors.
Thank you for stopping by.
This post was shared and voted inside the discord by the curators team of discovery-it
Join our community! hive-193212
Discovery-it is also a Witness, vote for us here
Delegate to us for passive income. Check our 80% fee-back Program
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider supporting our funding proposal, approving our witness (@stem.witness) or delegating to the @stemsocial account (for some ROI).
Please consider using the STEMsocial app app and including @stemsocial as a beneficiary to get a stronger support.