The Daily Life of Pathology Training
It's been a hectic life for the past three weeks and I'm glad I'm taking a short breather before the next round happens in less than six days. Just sharing some parts of my work routine and already giving you a warning that the images I use below might be too gross for some readers. They feature real human organs preserved in formalin and cut up for examination.
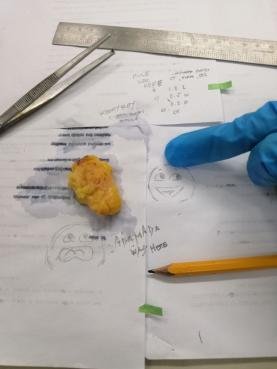
The above specimen is a Lipoma taken from the back of a patient that was left to grow for years
This is part of my Surgical Pathology exposure. The part of pathology training where we cut up specimen sent to us and process them for diagnosis. If you're familiar with Histology, you would know about the Hematoxylin and Eosin stains as a staple way to view different microscopic features of the specimen preserved on the slides.
The H and E stained slides are the basic slides used to examined the morphology. Most of the cases encountered can be diagnosed with these type of slides alone but for complex cases like the specimen having anaplastic/complex/bizarre forms, immunohistochemical stains are used to identify which possible organ is being viewed. For example, metastases can happen where lung cancer cells can travel to the liver but the form can't be distinguished easily so we have to use stains specific to detect ling tissues on liver specimens just to determine if the cells in question might have been from lung origin.
I'm just dumbing some pathology concepts down. I'm not exactly trying to be academic about it as I know we have too few users here who are medically inclined. It would be nice to have a community where conventional medicine was the subject. There I go ramble again.
The whole routine can be summed in a series of steps, acquisition of specimen, fixation/preservation, cutting of the specimen, fixation/preservation, slide review, sign out or do further studies. Each step in the process has their own set of rules and hassles to deal with.
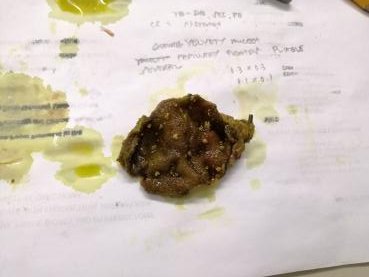
A gallbladder suffering from chronic cholecystitis with cholesterolosis. Those tiny yellow nodes on the inner surface can be mistaken for polyps on ultrasound. Sometimes I recover some stones while opening these.
Acquisition of the Specimen:
Specimen is sent to the Histopath Dept. for processing. Checks are done to verify whether it came from the right patient and completeness. Errors that can happen from this part include mislabeling the specimen or failing to account the specimen sent for completeness. It’s a touch move practice, as soon as you cut the specimen without checking for completeness, you might end up getting sued if you didn’t process everything claimed on the request. If there was no peritoneal fluid received but the request mentions it, you’re going to have a bad time when you processed the specimen and released the results forgetting a peritoneal fluid was supposed to be included.
Fixation and Preservation Part 1:
Some specimens take time to fix as they are taken out fresh. The ordinary formalin with 10% concentration can penetrate the tissues around 0.4cm per hour. For fatty specimens like breasts, it can take another 24 hours to process then after receiving as you have to cut some small slits to the tissue to aid with the formalin penetration.

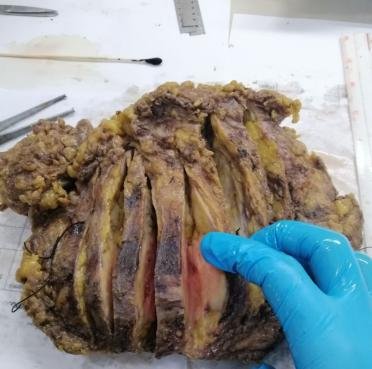
This is an entire breast on the back side view. You can see how much fat the specimen is. I had an entire day to have it fixed and the formalin still hasn't penetrated well. The blue stuff you see is the dye injected when it was trying to map for lymph nodes (sentinel lymph node biopsy).
Cutting the specimen:
Depending on the specimen, the technique to cut and how many times to sample will depend. The diagnosis in consideration also contributes to how hard the task would be. For cases like cancer, we would usually take more cut sections vs benign cases where it only requires few representative slides. There’s an art about the process as how often you have to change blades, gloves, and direction to slicing up the specimen matters.
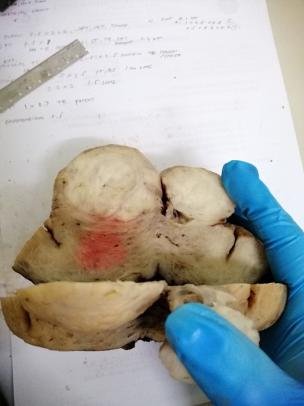
A different breast specimen but this time well preserved. You can see the difference in what a specimen looks like when it's ready for cutting. That pink stuff is where some of the formalin couldn't reach as it's been encapsulated by the tumor of interest.
Fixation and Preservation Part 2:
After being cut and sectioned into pieces, we got to label them by numbers and document which sections represent which part. The common errors here is mixing up the specimen parts by assigning different labels. You would be surprised to open a uterus tissue in a specimen labelled gallbladder if you F up this part. Never happened to me, yet. Some specimens take additional days to process, like fatty tissues from breasts and gallbladder, we put them in concentrated formalin (37%) compared to ordinary formalin (10%) to have better penetration and fixation. It depends on the nature of the specimen on which preservative jar we’re supposed to put it.
It's a uterus with a single intramural myoma on it. The red spot is where the preservative couldn't penetrate so it looks kinda fresh. I had the specimen fixed for a few days not really a problem since most of the parts have been penetrated by the formalin. We measure the depth of penetration of the tumor. It only looks like two different tumor but it's dissected in half.

This is just 1/20 of the amount of slides I had to read for the entire two week rotation. I had several towers stacked that using a slide box was no longer practical. Each slide can take up to several minutes just to examine those microscopic details.
Slide review:
Probably the most time consuming part of the process especially if you happen to handle a different case. Interesting case is a double meaning in our field, this means the case is complex that it can take weeks to figure out the diagnosis, or it can mean we can fulfill our required number cases to graduate. This is the double standard when working with complex cases, you can have a love and hate relationship with them. The slide review can be the quickest part of the process especially if it’s just a common case like appendicitis or cholecystitis. But for cancer cases, you may have to take more hours on textbooks to see if you get it right.
Sign out or further studies:
This is the part where you flex what you know with the consultant. If you got your diagnosis wrong, no shame, you’re still in training but it puts a dent on your impression with your seniors and consultants as you are judged based on your ability to keep up with the training. Sometimes even consultants have difficulty coming up with a diagnosis so they would have the specimen be passed around to other consultants for co-consultation. I think it’s a good way to gauge relationships between colleagues as you get extra help later on with this practice.
I’ll be rotating to Clinical Pathology soon. It's where the usual laboratory test results are being handled. This is where most clinicians can relate as we got some common ground on interpreting lab results. I might have rambled too much so I’ll end the blog here.
Posted with STEMGeeks
I see you’ve been doing some grossing. Nice.
I took that as two meanings. 1 being examining the specimen grossly for the findings to document and 2 being grossed out by the activity.
The smell of carcinogenic formalin killed my already dying sense of smell.
It's an acquired smell. You'll get used to it.
Congratulations @adamada.stem! You have completed the following achievement on the Hive blockchain and have been rewarded with new badge(s) :
Your next target is to reach 500 upvotes.
Your next target is to reach 100 upvotes.
You can view your badges on your board and compare yourself to others in the Ranking
If you no longer want to receive notifications, reply to this comment with the word
STOPSupport the HiveBuzz project. Vote for our proposal!
!discovery 15
This post was shared and voted inside the discord by the curators team of discovery-it
Join our community! hive-193212
Discovery-it is also a Witness, vote for us here
Delegate to us for passive income. Check our 80% fee-back Program