Sampling Technique and Errors Being a Pet Peeve
Let me just paint a common scenario:
A patient calls you over the phone asking why the results turned out non-diagnostic, inconclusive, or inadequate when everything else points to the obvious a lot. This patient had a lung mass and other imaging tests and biochemical tests had been run with results pointing to cancer. But why was the aspirated sample show only normal findings?
Because that’s just how the sample looked liked when it was processed and examined. You see, when clinicians that miss their mark sampled the wrong areas, it’s natural to send samples that don’t actually contain the cells of interest. It’s a simple and honest mistake but gets inflated because rather than admitting some fault, the clinician would just tell the patient the Pathologist read the sample wrong to save face.
Now from a Pathologist’s stand point, when those slides get reexamined for a second opinion, it’s hard to stick your neck out for a benign sample and then outright committing malignancy. You get a law suit for that but these things happen often and someone just has to take the fall to save a colleagues face. It took some time to pacify the irate patient but I could empathize their frustration after being told it’s normal when they were conditioned it wasn’t.
It's an ethical concern to bring up ideas like maybe your attending physician screwed up and missed their mark when they poked you for some samples. That's just asking for problems even if that's the most plausible explanation on the above case. You still have to maintain some good relations with your colleagues.
A second sampling was done with more CT guided and it turned out adenocarcinoma. Great, now the error has been fixed but sucks for the patient to solidify the bad news but that’s not what the post wants to highlight. The legal part of medicine is keeping a level head and making sure you commit to battles you’re sure you can win and can be confirmed by another observer objectively. At the end of the day, when months to years have passed, the only thing left with you are the slides you processed and these can be reviewed years after.
So when you got a benign sample after those slides are reviewed, what exactly does that legally look like if those samples can’t support your claim? Diagnosing cases aren’t easy, some samples can appear the same form under the microscope but can be caused by different lineages of cells you wouldn’t expect to be even present there. We do immunohistochemical stains, and molecular studies to narrow down these tricky cases but rarely do we go all out on the diagnostics due to the financial limitations the patient has.
Here’s a small idea of how the algorithm looks like simplified. The stains on the left side of the table are antibodies that target the specific antigens of interest. A dye/pigment is attached to the antibody and processed as soon as the binding is done to make it easier to spot under the microscope. The left most column are the stains that target the specific antigen.
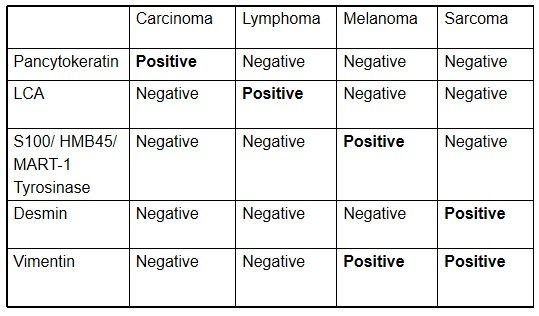
As you can see, if the cells stain positive for CK7 or CK20, or in different combinations, there’s a lot of diagnosis possible to eliminate. There are a lot of immuhistochemical stains and these are often pricey to opt for that’s why their use has become limited even if critically necessary in patient care but that’s a separate issue to deal with entirely. It takes some years of practice having these mentally memorized as you have to pair this up with experience. It always amazes me at how quick consultants tend to suggest specific stains to help them pin down their diagnosis on the fly.
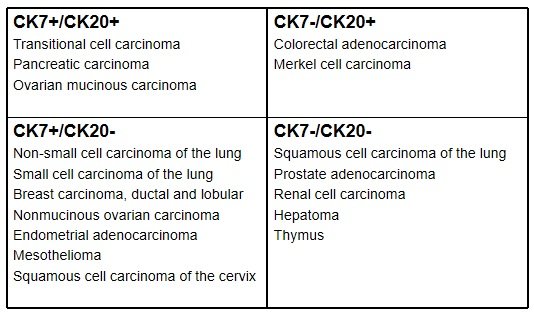
It’s also not a clear cut that if the disease in mind fits into the algorithm one can auto commit, some caution is needed as some aberrant forms can stain positive when you expect them to be negative by a small percentage of the time. So take the tables above as a general guide of what is usually observed as not all carcinomas stain with pancytokeratin.
If you made it this far reading, thank you for your time.
Posted with STEMGeeks
Interesting.
We always have handy little "cheat sheets" so we don't have to go off of memory on some things.
Worst case, we just go back and look at the SOPs.
We're expected to memorize the CK7/CK20 cheat sheet as this is like one of the alphabet in immunohistochemistry. It's not a hard rule as some aberrant expressions do happen when one stains positive when they're not supposed to which adds more complication to things. There's also a lot of stains out there and their algorithms are different. Just having a lymphoma panel is already a league of it's own. More updates on the method would have more organs and diseases staining behaviors and why this stain is no longer best stain which can be hard to keep up.
The last time I memorized a chart was biochemical reactions of different pathogens.
On the job, they are often underutilized knowledge compared to the stuff you had to memorize.
!discovery 20
This post was shared and voted inside the discord by the curators team of discovery-it
Join our community! hive-193212
Discovery-it is also a Witness, vote for us here
Delegate to us for passive income. Check our 80% fee-back Program
Congratulations @adamada.stem! You have completed the following achievement on the Hive blockchain and have been rewarded with new badge(s) :
Your next target is to reach 1750 upvotes.
You can view your badges on your board and compare yourself to others in the Ranking
If you no longer want to receive notifications, reply to this comment with the word
STOPCheck out the last post from @hivebuzz: