Getting a shot at the Squamocolumnar Junction
The specimen is a cervix. I’m just going to share an old pic to show what the cervix looks like when preserved in formalin below. The microscopic slides I’m using here are from a different specimen.

The lower part is the stratified squamous lining while the top part has the glands lined by simple columnar epithelium. Though this section shows a loose part owed to processing problems but not so bad that one can delineate the junction.
The cervix is the bottom most part of the specimen previously opened. That rough area is the part I would include in my sections to get the junction but not too high that I might sample the endometrium.
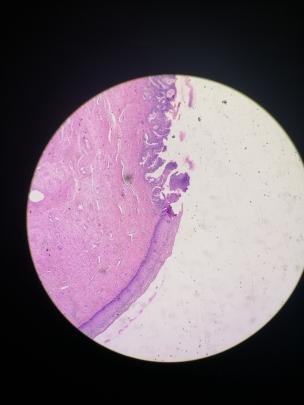
The squamocolumnar junction is that part of the cervix where the epithelial lining changes from the stratified nonkeratinizing squamous epithelium (outside) to simple columnar epithelium (inside). It’s significance is this being a hot zone for a lot of cancer especially HPV related. Pathologists would look at the zone if the cells start to look funny and invasive even on benign looking specimens.
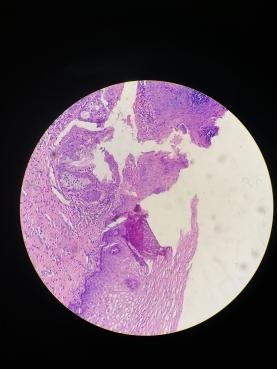
The hassle when processing the cervix when you can’t find this junction once the slides are processed. Grossly, it’s difficult to tell you’re cutting out the junction as it can only be confirmed microscopically so that means a slide not having the junction is an additional two or three days delay to sign out the case. It’s one of the most frustrating parts of processing the female reproductive system but not difficult, just dragging to do.
When cutting up the specimen, I would have to change gloves, the blades used, and also take extra sections for good measure. Sometimes the quality of your sections is not within your control especially when the specimen was poorly preserved or when the cervix has rubbed itself closely on the container’s sides scraping off the linings. Consultants would insist having this a prerequisite before signing out because it might cause legal complications like a missed diagnosis.
If you made it this far reading, thank you for your time.
Posted with STEMGeeks
Electronic-terrorism, voice to skull and neuro monitoring on Hive and Steem. You can ignore this, but your going to wish you didnt soon. This is happening whether you believe it or not. https://ecency.com/fyrstikken/@fairandbalanced/i-am-the-only-motherfucker-on-the-internet-pointing-to-a-direct-source-for-voice-to-skull-electronic-terrorism
Ahh the good ol’ container damaging the specimen ordeal.
I don’t envy the peeps in histology, etc.
We had all sorts of specimens being received. Like a breast part excised 2 weeks prior and only preserved in normal saline coming from a far flung area because some idiot thought that was enough as a preservative. Naturally opening that stuff meant smelling corpses submerged in saltwater for a long time. I don't know what goes on into these people that do this.
Some limbs sent include hands giving the middle finger because the orthosurgeon thought it was funny to leave it that while anticipating rigor mortis.
And finally some specimens (medium to large) get forcefully placed in an IV bottle and be attempted to seemingly soaked in formalin just cause they are too lazy to find a bigger container making some parts unpreserved.