The Importance of the Umbilical Cord (A Journey from Pregnancy to Childbirth)
Let's delve into the intricate process of fertilization and pregnancy. When sexual intercourse, or coitus, occurs, sperm enters the vagina, embarking on a remarkable journey towards the potential creation of life. These tiny swimmers move at a rate of 1 to 4 millimeters per minute, with the goal of reaching the egg for fertilization. Fertilization is most likely to happen during ovulation when changes in cervical mucus assist sperm in passing through the cervix and into the uterus. While this journey may seem simple and even enjoyable, sperm cells face numerous challenges along the way.
The female immune system recognizes sperm cells as foreign and at such attack them. At this point, lots of sperm cells are killed and those that survive get into the uterus. The pumping motion within the Uterus propels sperm cells towards the egg. Sperm is able to move, thanks to cilia which creates a sweeping motion for the sperm. On reaching the egg, an enzyme known as Hyaluronidase is released by the sperm in a process known as Acrosome biogenesis which help the sperm penetrate the egg's coats, thereby fertilizing the egg.
Following fertilization, the fertilized egg embarks on a journey down the Fallopian tube toward the uterus. Here, the process of implantation takes place. The embryo attaches to the uterine lining, triggering the proliferation of outer layer cells known as trophoblast cells. These cells lose their individual membranes and merge to form a single structure called Syncytiotrophoblast. This multi-nucleate cytoplasmic structure invades the uterine wall and begins secreting the hormone Human Chorionic Gonadotropin (hCG), a vital pregnancy hormone that plays a crucial role in maintaining the Corpus luteum.
Menstruation is stopped, thanks to the Corpus luteum which produces progesterone. The Hormone 'Human Chorionic Gonadotropin' helps to keep the corpus luteum until the placenta takes over hormone production. At the hospital, hCG is one marker used to detect pregnancy, as pregnancy test in hospitals as well as the home kits uses the presence of the hormone to ascertain a positive result in Urine or Blood.
Asides from determining if a woman is pregnant or not, elevated level of hCG is one factor for morning sickness in pregnant women which comes with symptoms such as nausea, vomiting, and tiredness. The hormone is also responsible for establishing immune tolerance as well as immune response to protect the fetus from being recognized as foreign in the mother's body. The hormone hCG plays an important role in the development of the fetal organs as well as tissues starting from the first trimester.
During the second week of development, lacunae start forming in the syncytiotrophoblast, creating spaces that coalesce to form a network filled with maternal blood from the damaged endometrium. Finger-like projections known as chorionic villi extend, allowing oxygen and nutrient-rich maternal blood to flow into the villi space. This process facilitates the exchange of substances across the placenta membrane into the fetal blood and removes waste products from the fetal blood. It also anchors the placenta securely to the uterine wall.
Attaching to the fetus is the umbilical cord which helps to transport nutrients and oxygen to the fetus and remove waste product from the fetus. The Umbilical cord possesses stem cells that has the ability to create new types of cells that the fetus would need for development. The placenta is fully formed at the end of the first trimester and it is functional at this point helping to exchanges substances, hormone production, and immune protection as it acts as a selective barrier to filter out toxins, pathogens, and drugs that could endanger the fetus. It also plays a role in regulating the fetus temperature ensuring a stable and enabling environment.
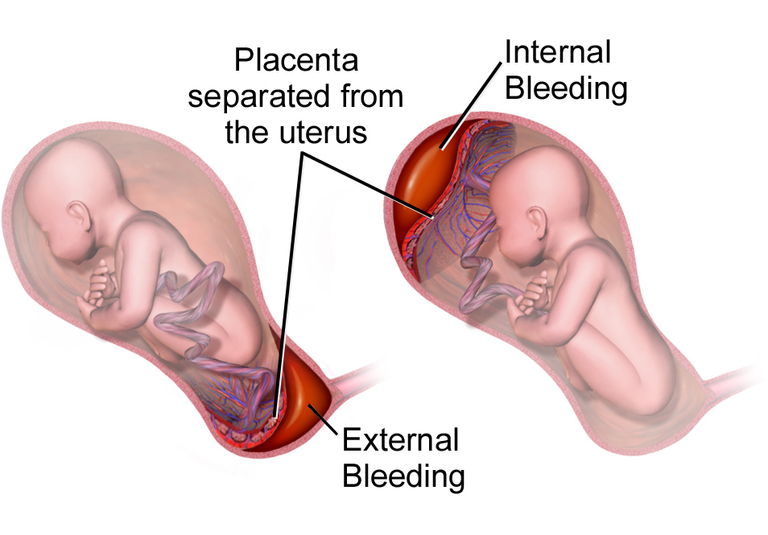
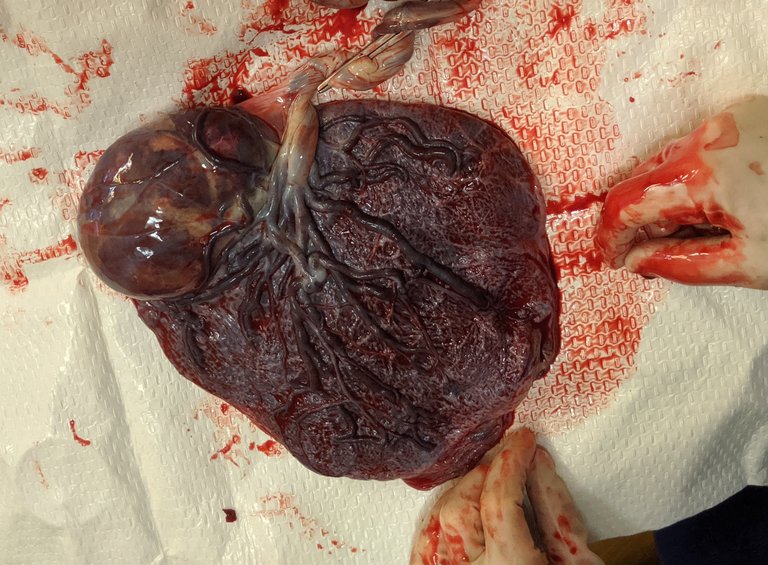
As delivery approaches, the placenta increases its hormone production, including prostaglandins, which play an important role in softening and thinning the cervix, preparing it for dilation and facilitating the onset of contractions leading to labor. The placenta stores enough oxygen and nutrients to sustain the baby even when blood flow is temporarily reduced during uterine contractions. Once the baby is delivered, the contraction of the uterus causes the placenta to detach from the uterine wall, and these contractions continue, known as afterbirth contractions, to completely remove the placenta from the uterine wall and expel it from the uterus.
Reference
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3271650/
https://www.ncbi.nlm.nih.gov/books/NBK26843/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4637467/
https://www.ncbi.nlm.nih.gov/books/NBK532950/
https://www.ncbi.nlm.nih.gov/books/NBK546679/
https://www.ncbi.nlm.nih.gov/books/NBK557389/
https://www.ncbi.nlm.nih.gov/books/NBK557490/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9536075/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6108594/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9325306/
https://www.sciencedirect.com/topics/medicine-and-dentistry/chorion-villus
Thanks for your contribution to the STEMsocial community. Feel free to join us on discord to get to know the rest of us!
Please consider delegating to the @stemsocial account (85% of the curation rewards are returned).
Thanks for including @stemsocial as a beneficiary, which gives you stronger support.